Bacterial pathogens affecting birds are numerous. This paper covers many of the species that affect companion birds and the antibiotics most commonly used to deal with them. Beneficial and harmful bacteria are discussed as well as the harmful effects of bacterial infections. Diagnostic testing with staining, cultures, histopathology, and cytology and explained.
Introduction
When people think of bacteria, they consider them just disease-causing organisms, but the vast majority of bacteria don’t cause disease. Rather, they play important roles in the environment and health of all living things, including humans and birds. They contribute to food and oxygen production. Neither plants nor animals could survive without bacteria.
Bacterial pathogens have existed for millennia. In past centuries, many remained in the hilly, forested lands around the world. In the past two centuries, however, as farm land was being developed and forests were torn down to make way for cities and buildings, many of the bacterial and viral pathogens lost their secret homes and went in search of new hosts to inhabit.
As long as these bacteria remained in the hills, forests, waterways, and farmland, they had no need to spread out. Many of the bacterial diseases that once were thought to be long gone and no longer a threat are recurring and persisting. Most occurred in Asia and Africa, where deforestation is rampant. Animals are also subject to illness from these pathogens. Before we delve into the bacteria that are most commonly found in birds, we will explore those frequently used antibiotics administered to avian species since there are references to them in the paper.
Part 1 The Role of Antibiotics in Avian Health
1.1 The Origin of Antibiotics
Bacteria are single-celled microorganisms that appear in many different metabolic types, geometric shapes, and environmental habitats. Some are beneficial for people and animals, and some are not. They can only be seen microscopically, and most have yet to be categorized.5
1.1.1 Sir Alexander Fleming and Penicillin
Humans have been using antibiotics for themselves and animals for decades, but these drugs have not been used for birds for nearly that long. Physicians and physicists have known since 1874 that “certain cultures of the mold, Penicillium glaucum, inhibited bacterial
contamination,” 6 but it wasn’t until 1928, when Sir Alexander Fleming identified what is known today as penicillin, that it was able to be used commercially. He found that molecules which were produced by certain molds killed or stopped the growth of specific bacteria. Fleming was doing research on a “culture of disease-causing bacteria when he noticed the spores of a green mold, Penicillium chrysogenum, in one of his culture plates.” 6 Fleming theorized that the mold must secrete an antibacterial substance, and he named it, “penicillin.” His work won him the Nobel Prize. It was first used during World War II, and soon after the war it was made available to the general public. Understanding the vast world of antibiotics and anti-infectives is no easy task. 13, 6

Image 1. Alexander Fleming, the discoverer of penicillin (image courtesy Biology Corner). https://www.biologycorner.com/worksheets/articles/alexander_fleming.html

Image 2. This mold, identified as Penicillium notatum, had inhibited the growth of a colony of Staphylococcal bacteria in the Petri dish (image courtesy YS journal.com via en.wikipedia.org.)
1.1.2 The Light Microscope
The microscope is the most important tool the avian veterinarian has for discovering the pathogens that are found in birds. It enables him to see the bacteria, fungi, protozoa, parasites, and viral inclusion bodies, many times without or before staining.
The light microscope employs visible light to small samples and is probably the most well-known and well-used research tool in biology. It is used to view samples with the available room light or with a light affixed to the microscope. The smallest objects that are considered to be living are bacteria, and even those may be observed and cell shape recognized at a mere 100x magnification. It is also called “Bright Field Microscopy.” 14
In optical or light microscopy, visible light is transmitted through or reflected from the sample through a single or multiple lenses to allow for magnification of the sample. This image may be seen directly by the eye, viewed on a photographic plate, or captured as a digital image. 14

Image 3. A stereo microscope
1.2 Classification of Antibacterial Medications and Their Functions
1.2.1 Antibiotic Classifications
Antimicrobials are medications that kill or stop the action of a bacterial pathogen. Antimicrobials are classified according to their function. Antibiotics are one class of antimicrobials; they fight against bacteria. Another class is anti-mycotic; these will stop fungal diseases. Anti-viral attack viruses, and anti-protozoal drugs fight protozoal diseases. Most antibiotics fall into their individual antibiotic classes. An antibiotic class is a grouping of different drugs that have similar chemical and pharmacologic properties. “Their chemical structures may look comparable, and drugs within the same class may kill the same or related bacteria.” 1
1.2.2 Broad- and Narrow-spectrum Antibiotics
Not all antibiotics work against all types of bacteria. Narrow-spectrum antibiotics are only effective against a limited range of bacteria; for example, penicillin G is very effective at killing gram-positive bacteria, but not very effective against gram-negative bacteria. Broad-spectrum antibiotics are effective against a wide range of bacteria. 16
What causes an antibiotic to have a narrow spectrum of antimicrobial activity? “Often, it has to do with the ability of the antibiotic to penetrate inside of the bacterium. Gram-positive bacteria have a relatively loose outer wall that many antibiotics can diffuse through. However, gram-negative bacteria have a complex outer layer that prevents the passage of many larger or fat-soluble molecules.” 16
Another reason that antibiotics can have a narrow spectrum of activity can be their target molecules. If an antibiotic targets a molecule that is not in the bacterium, it won’t be effective against that bacterium. For example, isoniazid specifically targets mycobacteria, the bacterium that causes tuberculosis. It’s specific because it prevents the synthesis of mycolic acids, which are found in the cell walls of mycobacteria, but not most other types of bacteria. 16
If the patient is treated with an antibiotic that has a narrow spectrum of activity, the ‘good’ bacteria that normally live inside the body won’t all get destroyed along with the pathogen that caused the infection. However, it is not always clear which microbe is causing the illness; therefore, the patient will be started on a broad-spectrum antibiotic so that the medication can work quickly and the patient can survive until the specific bacterium is determined and the more appropriate antibiotic is prescribed. 16
1.3 Bactericidal and Bacteriostatic Antibiotics
Antibiotics are generally divided into two groups based on their method of action. They either kill bacteria or prevent them from growing. They are prescribed when there is an infection that the body’s immune system is unable to deal with. Antibiotics that kill bacteria directly are called “bactericidal,” which means “kill bacteria,” and those that stop bacteria from growing are called “bacteriostatic,” or “staying stable.”. 16

Image 4. The difference between bactericidal and bacteriostatic medications’ effect on bacteria in a laboratory setting (image courtesy Slide Share). https://www.slideshare.net/kyawsanlin25/terminologies-on-anti-infective-agents
FREE Training to Stop Your Bird's Biting
Get FREE access to Beak School – the only system designed to train your bird. Stop behavioral problems like biting, screaming, feather plucking.
Get the Free Training1.3.1 The Mechanism of Bactericidal Antibiotics
The different antibiotics have different mechanisms. For example, “the antibiotic polymyxin B injures the plasma membrane of bacteria, allowing their contents to leak out of the cell wall. Under normal circumstances, bacteria and other cells have to keep a perfect balance of ions on both sides of the plasma membrane because of osmosis. Polymyxin B disrupts this balance and also lets other important molecules, like DNA and RNA, leak out, and so the bacterium is destroyed.” 7 Other bactericidal antibiotics include vancomycin, metronidazole, aminoglycosides, fluoroquinolones, penicillin, and cephalosporins. 16 The minimum concentration of a drug that is needed to kill a certain strain of bacteria is called the “minimum bactericidal concentration” or MBC. 16
1.3.2 The Mechanism of Bacteriostatic Antibiotics
In contrast to bactericidal antibiotics, bacteriostatic antibiotics inhibit the growth of the bacteria. The bacteria don’t die, but neither can they grow or replicate. Unlike the bactericidal agents, when bacteriostatic agents are used, microorganisms remain viable, and their numbers remain the same. Bacteria normally divide really quickly in the body, and their numbers can quickly get out of control. Bacteriostatic antibiotics stop them from growing and dividing, so the host’s immune system will then be able to take over and destroy the harmful bacteria. 16
Bacteriostatic agents are used to limit the growth and reproduction of microorganisms by interfering with their protein production, DNA replication, or other aspects of bacterial cellular metabolism. Unlike the bactericidal agents, the bacteriostatic agents must work together with the immune system to inhibit the microorganism’s activities. According to drug concentration, the activity may vary. For example, if high concentrations of bacteriostatic agents are used, they may kill the bacteria, whereas low concentration of bactericidal agents may simply inhibit their growth. Tetracycline, sulfonamides, spectinomycin, trimethoprim, chloramphenicol, macrolides and lincosamides are some examples of bacteriostatic agents. Minimum concentration of a drug that is needed to inhibit the growth of a certain strain of bacteria is known as “minimum inhibitory concentration” or MIC. 16
Tetracycline is an example of a bacteriostatic antibiotic. It inhibits the bacterial ribosomes so that no new proteins can be made. This doesn’t kill the bacteria; they already have the proteins they need to survive for a while. However, they can’t replicate because they would need to make many new proteins in order to make a whole new bacterial cell. Other bacteriostatic antibiotics include chloramphenicol, trimethoprim, clindamycin, sulfamethoxazole, and erythromycin. 16
1.4 Determining Factors When Choosing an Antibiotic
In some cases, there may be multiple bacteria present. One antibiotic might kill one strain but only inhibit the growth of another. It is for this reason that the veterinarian may choose to use two different antibiotics. The practitioner needs to know all aspects of the bacteria and the antibiotics he wishes to use before making his choices. He may choose one or both types when treating an infection. His choice depends on:
- The type of infection
- Growth conditions of the microorganisms
- Bacterial density
- Test duration, and the
- Reduction rate of the bacteria.48
In most cases of antibiotic use, a doctor must choose an antibiotic based on the most likely cause of the infection. For instance, if the bird has a skin infection, the doctor needs to know which antibiotic to prescribe for skin infections, and he will prescribe the best antibiotic for that type of bacteria. 8, 48
1.4.1 Testing to Determine Antibiotic Sensitivity
Laboratory tests may be required for the veterinarian to choose the proper medication. Gram’s stains can be used to identify bacteria under the microscope; these will also tell him which bacteria are present and provide information he needs to choose the proper antibiotic. Certain bacterial species will take a stain, and others will not. Those that don’t will be examined directly under the microscope. Many times, the veterinarian will do both—direct and stained microscopic analysis. 48

Image 5. Bacteriology plate showing the antibiotic sensitivity. “The best antibiotic to use is the one which leaves a clear ring around the antibiotic disk. This is how we choose which drug will work best in a difficult situation” (image courtesy Michael J. Cannon) 13
The veterinarian may need to do a culture on a bacterial sample which is allowed to grow in a laboratory. The results may take a few days to come back from the lab. The way bacteria grow or what they look like when they grow will help to identify the bacterial species. Cultures may also be tested to determine antibiotic sensitivities. “A sensitivity list is the roster of antibiotics that kills a particular bacterial type.” 48 This list will confirm that the correct antibiotic is being dispensed. Treatment is based on the location of the infection and the results of the culture-and-sensitivity testing. 48
1.4.2 Other Considerations When Choosing an Antibiotic
The practitioner must also consider the species he’s dealing with. Songbirds, canaries and finches, poultry, and psittacines all belong to different taxonomic orders. They react differently to medications, and this needs to be taken into consideration by the veterinarian. The practitioner must consider other factors when choosing an antibiotic: medication costs, dosing schedule, and common side effects are often taken into account. He must also consider how the bird reacts to a specific antibiotic; if there is a negative reaction, he will have to change to a different antibiotic. In some aviaries or households with multiple birds, and if the infection is transmittable to other birds, all the birds may need to receive the antibiotic. If it is a zoonotic disease (transmittable to humans), the clinician will advise the owner to see his own physician. 48
A very important question the veterinarian must ask the client concerns the owner’s comfort level with giving the bird the medication. Some people are really confident with syringing medications into the bird or giving injections, and others simply can’t bring themselves to do it. For those who feel they are unable to give their bird the needed medication, the veterinarian might choose to give the bird a long-acting injection in the office if the antibiotic comes in an injectable form. This way, the owner might not have to administer medication himself. Sometimes the veterinarian will begin with a fast-acting injection, and the client will need to continue the treatment with oral medication at home. 48
1.4.3 Incorrect Antibiotic Usage in Birds
Even though antibiotics are used quite commonly in aviculture, many owners are confused about how they work and how they are used. If they are not used correctly, or the bird develops a resistance to it, the drug may not work at all. This is often a major problem, since if either is the case, the drug may be of no use to the patient. 13
The purpose of using an antibiotic is for the bird to develop “strong, adequate levels of the drug in the bloodstream.” 13 The blood’s job is to carry the antibiotic to the infected area of the body. If the dose of the antibiotic is too low, or if it is not given frequently enough, it will fail to work. In addition, if the antibiotic is not used correctly, the bird may develop a resistance to the drug, and other birds in the home or aviary may be at risk of contracting the disease. 13
Due to the misuse and overuse of antibiotics, some people have a negative opinion about antibiotics, both for themselves and their pets. This negativity is unfounded; antibiotics are extremely valuable medications. Antibiotics have changed medicine for the better, having been instrumental in curing such infectious diseases as pneumonia and tuberculosis. When used correctly, they are a vital tool for the practitioner. 6.
1.4.4 Correct Use of Antibiotics in Birds
The antibiotic’s purpose is to kill bacteria; however, they do not all work the same way. Some kill gram-positive bacteria, while others kill gram-negative bacteria. Most gram-negative bacteria are harmful, and most gram-positive bacteria are beneficial and are normally in the body; however, there are some very dangerous gram-positive bacteria out there. Since penicillin has come on the market, there have been many new classes of antibiotics created to deal with the different strains of bacteria. For example, fluoroquinolones such as enrofloxacin (Baytril) are used extensively by avian veterinarians. Giving the wrong antibiotic for a specific bacteria will either be ineffective, or worse yet, cause the infection to worsen 7
Antibiotics must be given for a prescribed period of time. Doctors and veterinarians prescribe for a specific amount of time because research data supports that it takes this much time to adequately kill an invading pathogen. So, if people do not comply with giving their birds the entire course because the bird seems to be improving, they risk the possibility that some of the more resistant bacteria are still in the bird’s system. Bacteria can mutate and develop a resistance to the antibiotic. Then the veterinarian has to use stronger antibiotics. Sometimes these work and sometimes they don’t. This can result in an even more virulent infection soon after. If none of these stronger drugs works, the bird may succumb to the infection. 7
1.5 Antibiotic Drugs and Their Usages
1.5.1 Table of Commonly Used Antibiotic Drugs
|
Penicillin |
They are used for several types of infections like urinary tract infections, respiratory infections, and skin infections. |
|
Cephalosporins |
They treat a wide range of infections as well as serious infections like meningitis and septicemia (presence of disease-causing bacteria in the blood). |
|
Aminoglycosides |
These are mostly and generally used only to treat serious conditions like septicemia due to their severe side effects such as kidney damage. Also, they have to be injected because they can easily break down in the digestion system. |
|
Tetracyclines |
A broad-based antibiotic used to treat a wide range of infections. |
|
Macrolides |
A good substitute for penicillin, it is often used for patients who are allergic to penicillin or have bacteria that are resistant to penicillin. Diseases like lung infections can be cured by this medicine. |
|
Fluoroquinolones |
Broad-spectrum antibiotics that treat a wide variety of infections. 8 |
1.5.2 Antibiotic Nomenclature and Tradenames
Most antibiotics have two names: the trade or brand name, created by the drug company that manufactures the drug, and a generic name, based on the antibiotic’s chemical structure or chemical class. Each antibiotic is effective only for certain types of infections. Although there are well over 100 antibiotics on the market, the majority come from only a few types of drugs. These are the main classes of antibiotics: 1
- Penicillins, such as penicillin and amoxicillin
- Cephalosporins, such as cephalexin (Keflex)
- Macrolides, such as erythromycin (E-Mycin), clarithromycin (Biaxin), and azithromycin (Zithromax)
- Fluoroquinolones, such as ciprofolxacin (Cipro), levofloxacin (Levaquin), and ofloxacin (Floxin)
- Sulfonamides, such as co-trimoxazole (Bactrim) and trimethoprim (Proloprim)
- Tetracyclines, such as tetracycline (Sumycin, Panmycin) and doxycycline (Vibramycin)
- Aminoglycosides, such as gentamicin (Garamycin) and tobramycin (Tobrex)
- Carbapenems, such as imipenem and meropenem
- Glycopeptides, such as vancomycin and teicoplanin
- Lyncomycins (such as Lincocin) 1, 48
1.5.3 Over-the-counter Antibiotics
Many owners decide to save money by purchasing antibiotics from a pet store. Since the owner is unable to diagnose his bird properly, these do little to no good. These water-based medications are so broad-spectrum that they are not effective against a specific bacterium. The bird’s illness cannot be diagnosed without a veterinary exam and culture. Giving these medications causes the owner to waste valuable time in getting the bird the proper medical care. The sick bird’s condition deteriorates quickly—within hours even—once the infection takes hold. Time is of the essence when it comes to getting treatment for sick birds. 6
1.5.4 Antibiotic Interaction with Other Drugs and Foods
Many humans use home remedies that seem to work for them, but they should not use them on their birds. They are experimenting and that’s never a good idea. Birds are not mammals. What works on us does not necessarily work for them. It is especially important that they not give their bird home remedies during antibiotic therapy. Some foods can inhibit the efficacy of these drugs. Do not add grapefruit seed extract (GSE) to your bird’s water as an extra med when you are giving them antibiotics. Grapefruit is one of the foods that is well known by doctors to interfere with the absorption of some antibiotics. “Natural” is not by definition safe (not that GSE is natural–it is filled with preservatives). And don’t administer apple cider vinegar thinking it’s a cure-all for birds. It is only used for fungal disease, and even then it is just a temporary fix. The illness will not go away because of its use. It must be treated with the correct medication from the avian veterinarian. 7
1.6 Bacterial Resistance to Antibiotics
Antibiotics are typically used to treat bacterial infections. However, in recent years, the improper or unnecessary use of antibiotics has promoted the spread of several strains of antibiotic-resistant bacteria. With antibiotic resistance, infectious bacteria have built up a tolerance for antibiotics that had previously been effective. One such problematic bacterial strain is methicillin-resistant S. aureus (MRSA), a gram-positive bacterium, which resists methicillin and other antibiotics used to treat Staphylococcus infections. It has been found in birds and is quickly fatal. It spreads primarily through skin contact and causes skin infections. 54
Some pathogenic bacteria become resistant to antibiotics over time due to mutation. They may work for a while then cease to work after a time. As they change, it becomes more and more difficult to destroy them. This image demonstrates the effect the antibiotic has on bacterial cultures in which it has failed to kill the bacteria. 54

Image 6. Antibiotic-resistant strains of Staphylococcus aureus bacteria and Methicillin-resistant S. aureus or MRSA have become the most common cause of skin infections and are frequently found in birds (image courtesy Anthony Komaroff). https://www.askdoctork.com/mrsa-dangerous-201502037412

Image 7. An antibiotic’s effect on various bacteria (image courtesy 123rf). https://www.123rf.com/stock-photo/bacteria_culture.html?mediapopup=47047441)
1.7 Antimicrobials/Antibiotics Commonly Used in Pet Birds
These are commonly administered to avian patients:
Amikacin sulfate
Amoxicillin/clavulanate
Azithromycin
Ceftazidime sodium
Ciprofloxacin
Clindamycin
Doxycycline
Doxycycline injectable, 20 mg/mL
Enrofloxacin
Metronidazole
Marbofloxacin
Trimethoprim/sulfamethoxazole 6
1.8 The Use of Probiotics for Avian Patients
Although most antibiotics do kill the good bacteria as well as the harmful ones, most healthy birds will rebuild their supply of normal flora once the infection has cleared up and the bird returns to its usual diet. Owners may wish to give their birds probiotics–lactose-based bacteria that are used by humans to rebuild healthy flora. They are for the most part harmless; however, they are also a waste of money unless probiotics without lactose and made specifically for birds can be found. 7 “There is only one good probiotic out there, Sivoy, and it is made in Italy. So, most people will not be able to get it.” (However, Visbiome Vet is available here and is related to Sivoy. Ask your avian veterinarian about it) (R. Dahlhausen, personal communication).
Probiotics made for humans are specific for mammalian flora. Research into developing a true probiotic specifically for birds has been too expensive for most drug companies to pursue. It would have to be cultivated from birds, most likely chickens. Research on human probiotics can be translated from other mammals to humans, but not from mammals to birds. Birds are simply too different. 7
The development of antibiotics has changed the course of veterinary medicine. Since their use, countless numbers of birds and other animals have been saved from death by previously fatal diseases and infections. Ongoing research and development of new antibiotic drugs to combat these illnesses is vital.
1.9 Administering Medications Orally
Oral medications must be given directly into the mouth with an oral syringe. Putting them in the water is not a good idea. How much is the bird drinking? Is he drinking less because the water tastes unpleasant to him? Is he drinking more because he is overly thirsty and therefore getting too much medication? The only way to truly determine if your bird is getting the exact, correct dosage is to give it orally. As with children, it can be a struggle with some birds, but it is worth the effort to know he is receiving the correct dosage.7
Choose the correct size of oral syringe for the bird. Small birds should receive it from a .5 cc. syringe; medium-sized birds should take it from a 1 cc syringe, and larger birds can use a 1 cc to 5 cc syringe, depending on how well they take the medication. Some large birds are very difficult to dose, so a smaller syringe might have a better chance of getting the medication into them without so much waste. Be aware that you cannot skip dosages without jeopardizing the treatment plan. They must be given as directed by the clinician.
Part II What Are Bacteria and How Do They Work?
2.1 What are Bacteria?
Bacteria are microscopic, single-celled organisms with a simple internal structure that thrive in diverse environments. They can live within soil, in the ocean, and inside the human intestinal system. They contain ribosomes, spherical units within the cell where proteins are assembled from individual amino acids. 54
They can be beneficial, as in aiding in digestion, or harmful, causing disease, and they can survive in extreme environments due to their diverse metabolisms. Their ways of obtaining energy for growth and life have allowed them to colonize nearly every environment on earth.31 Not all bacteria are capable of causing disease, but each group has at least some disease-causing representatives. 39

Image 8. Ribosomes within the cell (image courtesy Billy Cell City). http://billycellcity.blogspot.com/2009/11/ribosomes-brick-factory.html
2.2 The Difference Between Aerobic and Anaerobic Bacteria
Bacteria may be divided into those which are aerobic and those which are anaerobic.
|
AEROBIC BACTERIA |
ANAEROBIC BACTERIA |
|
Are able to live in oxygen environments |
Can live without the presence of oxygen |
|
Can detoxify oxygen |
Cannot sufficiently break down food molecules as well as aerobic bacteria. |
|
Require food for its energy |
Can survive in places where there is less oxygen, such as intestinal systems. Some also cause diseases in those less oxygenated areas |
|
Cannot grow without an ample supply of oxygen involved in a chemical reaction |
Can grow without oxygen |
|
Employs aerobic respiration in order to use oxygen for cellular respiration |
Employs anaerobic respiration which has a less efficient energy cycle |
|
Uses aerobic respiration as energy produced by the complex process of oxygen and glucose metabolization within the cell’s mitochondria. |
Uses respiration as a product of fermentation |
|
Uses the oxygen present in the air for energy metabolism |
Does not need oxygen for energy metabolism |
|
In a culture, aerobic bacteria will gather on top to inhale most of the oxygen in order to survive |
In a culture, anaerobic bacteria will collect on the bottom to avoid the oxygen. |
|
All animals and humans are obligate aerobes that require oxygen for respiration |
Anaerobic yeast is an example of facultative anaerobe bacteria |
(Table courtesy Jilani) 29
2.3 Bacterial Structure
Bacteria range in size from 1 to 10 micrometers in length and cannot be seen without a microscope. They have no nucleus, and their genomes are a single circle of DNA.3 On the outside, bacterial cells are usually surrounded by two protective coverings: an outer cell wall and an inner cell membrane. However, some bacteria do not have a cell wall at all, and others may even have a third, outermost protective layer called the “capsule.” 54
Bacteria can move in a variety of ways. A number of them move about by secreting a slime that allows them to glide over the cell’s surface so that they slide through their environment. Others have flagella—small, whip-like appendages made of protein which move the bacterium along in a swimming motion. There are those that use pili, hair-like structures, which help the bacterium attach to the host surface. These aid them in “swishing through their watery environments.” 31

Image 9. Structure of a bacterium cell (image courtesy Montana Science Partnership). Science Partners.info, http://www.sciencepartners.info/module-3-soils/the-tree-of-life-part-1/bacteria
2.4 Bacterial Reproduction
Most bacteria multiply by binary fission. A single bacterial cell, the “parent,” makes a copy of its DNA and grows large in size by doubling its cellular content. The doubled contents are pushed out to either end of the cell. Then a small fissure emerges at the center of the parent, eventually splitting it into two identical “daughter” cells. Some bacterial species reproduce by budding. During budding, the daughter cell grows as an offshoot of the parent. It starts off as a small nub, grows until it is the same size as its parent, and splits off.31

Image 10. Pseudomonas fluoresences reproduces through binary fission. The bacteria splits apart, making almost an exact replica of the parent. Depending on the bacteria’s reproduction rate, there could be thousands of that bacteria produced in a day (image courtesy Site for Science). https://sites.google.com/site/sassiteforscience/standard-2/objective-d

Image 11. Reproduction by budding (image courtesy mr-roes in Wikispaces).
http://mr-roes.wikispaces.com/Asexual+Reproduction+Webquest
http://fpgeetutor.blogspot.com/2015/02/microbiology-principles-of-microbial.html

Image 12. Reproduction through binary fission (image credit mr-roes). http://mr-roes.wikispaces.com/Asexual+Reproduction+Webquest
2.5 Bacterial Classification and Shape
Bacteria come in many different sizes and shapes, and they are classified by their morphology, or shape and appearance. They can also be distinguished by the nature of their cell walls and by differences in their genetic makeup. 4, 7 The three basic shapes of bacteria are: 39, 54

Image 13. Normal cocci and fungal spores in a Gram’s stain swab; the small dots (black arrow) are the cocci and the large smears (red arrow) are fungal spores (image courtesy Bob Dahlhausen; used with permission)
2.5.1 Spherical or Round.
Round bacteria are referred to as cocci (singular, coccus). Cocci can also take their form in different configurations depending on the bacterium and environmental conditions. They can appear as:
- a single bacterium
- combinations of two (diplococcus);
- a linear chain, as in streptococcus;
- a cluster, such as in staphylococcus.
Cocci cause many illnesses Among the more common cocci is Staphylococcus aureus, which appears as a cluster of cocci. S. aureus often grows harmlessly on the skin, but given a chance, can do great damage to the bird’s skin or respiratory system. 39, 54

Image 14. Staphylococcus aureus
Staphylococcus (pl. Staphylococci) is a genus of spherical, gram-positive bacteria which occur in grape-like clusters (image courtesy “Go Pets America”). http://www.gopetsamerica.com/bio/bacteria/staphylococcus.aspx
2.5.2 Rod-shaped or Cylindrical
Cylindrical, rod-shaped bacteria are called bacilli (singular, bacillus). They occur singly or in linked chains. Escherichia coli is a rod-shaped bacterium that normally lives in the intestinal tract without causing disease; however, it can be harmful at other sites, such as in the urinary tract or on the skin. Some strains of E. coli are spread by contaminated food or water. 39 54 56
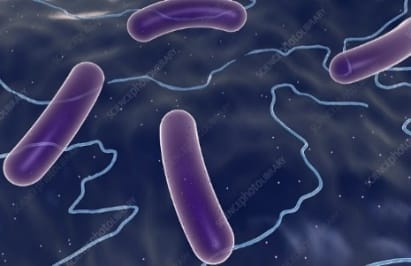
Image 15. Rod-shaped bacteria. A stylized scanning electron microscopic image of rod shaped bacteria (bacilli). Tetanus, anthrax and botulism are all caused by such bacteria.. (image courtesy Science Photo Library). https://www.sciencephoto.com/keyword/landscape).
2.5.3 Spiral
Spiral or spirilla (singular, spirillum) are rigid, corkscrew-like, spiral-shaped bacteria which can be further categorized depending on how much spiraling they show.39 One such bacterium is Campylobacter which is commonly found in raw poultry. Spiral bacteria can be sub-classified by the number of twists per cell, cell thickness, cell flexibility, and motility. The two types of spiral cells are spirillum and spirochete, with spirillum being rigid with external flagella, and spirochetes being flexible with internal flagella. 39, 47, 54

Image 16. Spiral-shaped campylobacter bacteria (image courtesy “Food Safety Magazine”). https://www.foodsafetymagazine.com/magazine-archive1/aprilmay-2010/control-of-salmonella-campylobacter-and-other-bacteria-in-raw-poultry/
The shapes and configurations of bacteria are often reflected in their names. For example, the milk-curdling Lactobacillus acidophilus are bacilli, and pneumonia-causing Streptococcus pneumoniae are a chain of cocci. 54

Image 17: The shapes of bacteria (image courtesy “Slideshare.net”). https://www.bing.com/images/search?view=detailV2&ccid=tw7N4wfv&id=3C37A9DE538B98626059F8943E8F8B6CC56DC8C4&thid=OIP.tw7N4wfvzpPcJcsy2Khu7AEsDh&q=different+types+of+bacteria&simid=608030189621480002&selectedIndex=9&ajaxhist=0
Part III Beneficial and Harmful Bacteria
3.1 Commensal Bacteria: Beneficial
There are many bacteria in the body that are important to health; they protect the host from disease-causing pathogens. 31
Commensal bacteria, which are Gram-positive, are usually beneficial. These are commonly found microflora which consist of those microorganisms which live on body parts covered by epithelial cells and are exposed to the external environment, such as the skin and gastrointestinal and respiratory tracts. Some of these bacteria, given the right conditions, can multiply so quickly that they overpower the immune system and become pathogenic, even though ordinarily they are beneficial. The most abundant bacteria are present in the lower part of the intestinal system, and most intestinal bacteria are Gram-negative anaerobes (organisms that live without oxygen). If allowed to multiply to high numbers, these can become pathogenic and will activate the immune system. If the immune system overreacts to these bacteria, there is the risk of inflammation.52
3.1.1 Normal Flora in the Bird’s Body
Any time a bird is ill, bacterial disease should be considered in the list of differential diagnoses (DDx). They are common in pet birds, and almost always due to poor husbandry and nutrition. Neonates and young birds are especially vulnerable. The most commonly found infections are gastrointestinal (GI) and respiratory. These can lead to systemic disease. Normal bacterial flora exist in all companion birds; in small numbers they do not produce disease, but when allowed to grow, they are very dangerous. 26

Image 18. Normal flora in choanal Gram’s stain in author’s cockatiel #1 (image courtesy Bob Dahlhausen; used with permission).

Image 19. Normal flora in choanal Gram’s stain author’s cockatiel #2 (image courtesy Bob Dahlhausen; used with permission).

Image 20. On the fecal Gram stain, author’s cockatiel #1 exhibited an overgrowth of normal bacterial flora. This is indicative of an intestinal imbalance and indigestion (image courtesy Bob Dahlhausen; used with permission).

Image 21. On the fecal gram stain, the author’s cockatiel #2 exhibited a normal number of gram-negative rods; see black arrows (image courtesy Bob Dahlhausen; used with permission).
Normal gut flora in adult psittacines is about 80-100% Gram-positive bacteria, and 0-25% of that is E. coli. Other Gram-positive bacteria found in the psittacine intestine consist of fecal Streptococcus, Staphylococcus, Lactobacillus, and Corynebacterium, to name a few. 49
Bacterial infections are common in pet birds, and clinicians should consider them when encountering illness in a bird. Gastrointestinal and respiratory infections are the most frequently seen and can lead to systemic disease. 26.
3.2 General Overview of Pathogenic Bacteria
Bacteria are single-celled microorganisms that lack a nuclear membrane, are metabolically active, and divide by binary fission. They are a major cause of disease in birds. Bacteria may seem to be simple forms of life, but in fact they are “sophisticated and highly adaptable.” 35
Most bacteria are able to multiply very quickly and can live for a long time on a wide variety of surfaces. These organisms exist in everywhere in both parasitic and free-living forms. 26
In general, the bacteria which invade bird species and cause disease are related to the feeding habits of that species. Since most psittacine species are primarily granivorous, their intestinal flora is predominantly Gram-positive. When bacterial disease is observed in parrots and other genera, it is usually, but not always, Gram-negative in nature. 44
The intestinal tracts of most healthy birds will contain potentially harmful bacteria. As long as these are small in number, they do not present a problem. But they can grow to larger numbers and create illness when the bird is stressed or immune-compromised, particularly if it is already fighting a concurrent illness.32 The droppings may change from normal color to very green (biliverdinuria) and become watery due to damage to the digestive tract, kidneys and liver. 34
Bacterial inhalation from dust in the air may produce sneezing, eye rubbing, excessive swallowing, yawning and gaping, coughing, and loss or change in vocalizations. Both inhaled and ingested bacterial infections are potentially life-threatening when left unattended. 34.
3.2.1 Obligate, Opportunistic, and Accidental Pathogens
In order to understand the means of identifying pathogens, one must know the types of pathogens that exist. The three categories of bacterial pathogens are:
- Obligate bacteria. This type must cause disease in order to be transmitted from one host to another. They must also infect a host in order to survive, in contrast to other bacteria that are capable of survival outside of a host. Examples of obligate bacterial pathogens include Mycobacterium tuberculosis and Treponema pallidum. 19
- Opportunistic bacteria. These takes advantage of an opportunity to cause disease. Opportunistic conditions allow the microorganism to activate, begin to multiply, and overwhelm the body’s weakened immune system.19 Opportunistic bacteria can be transmitted from one host to another without having to cause disease. However, in a host whose immune system is not functioning properly, the bacteria can cause an infection that leads to a disease. In those cases, the disease can help the bacteria spread to another host. Examples of opportunistic bacteria include Vibrio cholerae and Pseudomonas aeruginosa. 19
- Accidental bacteria. Some bacterial pathogens cause disease only accidentally. Indeed, the disease actually limits the spread of the bacteria to another host. Examples of these “accidental” pathogens include Neisseria meningitides and Bacteroides fragilis. 19
Most pathogens are Gram-negative, although some are Gram positive. Many pathogens, or harmful bacteria, can exist without causing disease if the numbers are low enough. However, if the numbers increase, they can cause serious diseases and infections such as meningitis, encephalitis, and myelitis. These bacteria include Salmonella, Listeria, S. aureus, Pseudomonas, Klebsiella, Mycobacterium, Streptococcus, Clostridium, and E. coli. These microbes are found everywhere in the environment. 18
3.2.2 Pathogenic Bacteria Must Be Able to Perform Three Actions:
- They must be able to enter and colonize the body. This happens when the person or animal breaths, eats, or drinks. They can enter through a wound or be passed on through sexual contact. They can also be passed on by parasites which bite an infected individual and then bite another, causing the same disease. 31
- They must overcome the body’s defenses. An immune-competent individual is usually able to throw them off, but if a person or animal is immune-compromised, the bacteria will be able to take over. Weakened immunity allows pathogens to reproduce rapidly and thus lead to any number of infections. 31
- They must damage the body. Pathogens produce toxins and enzymes that damage the body’s tissues. If food is improperly processed or cooked, or allowed to be out of the refrigerator too long, bacterial toxins can be become part of the food. Clostridium botulinum (botulism) is one such bacteria, often caused by improper canning methods. The toxins, not the bacteria, are what cause disease. 31

Image 22. Clostridia bacteria. These are the lines appearing on the image (black arrow) (image courtesy Sandhill Veterinary Services; used with permission). http://www.sandhillvet.co.uk/html/pigeon_service_management_diseases.html
3.3 Causes of Some Bacterial Infections
E.coli Contaminated food old fruit, fluctuating temperatures, draught, stress, wet areas, fungus infection, dirty cages
Streptococcus Cold stress, underlying viral infection, dusty environment, poor seed, stress
Staphylococcus Dust, mice, stress, poor seed, contaminated air conditioning, or dusty environment
Diplococcus Mice, stress
Citrobacter Poor water hygiene
Pseudomonas Poor water hygiene (e.g. bathroom grout and seal around sink) 56
3.4 Transmission of Bacterial Infection.
Droplet infection occurs when the person with a cold coughs and sneezes and large numbers of the particles become airborne. The particles contaminate everything they touch, including the bird itself and its surroundings. Infection is due to inhalation or ingestion of the bacteria. Many people allow the bird to come in contact with their mouths; this is dangerous as we carry many bacteria in our mouths that are normal for us but harmful to the bird, such as E. coli. 19
3.5 Symptoms of Bacterial Infection
“The trachea of a bird connects and seals to the sinuses through the choanal slit when the bird closes its mouth. Signs of upper respiratory or sinus infection are sneezing and nasal discharge. Tail-bobbing and difficulty breathing are due to either middle airway (trachea) or lower airway (lungs or air sac) disease. Birds with a severe upper (sinus) airway disease rarely show much difficulty in getting air in and out of the air sacs and through the lungs. They also don’t usually show systemic signs of illness until and unless the infection extends down into the middle or lower parts of the respiratory system. Their sinuses produce a wet, gurgly sound when their mouths are closed.” 19
3.6 Types of Bacterial infections
Symptoms depend on the part of the body infected and the severity of the infection. The disease can be peracute or chronic.
- Peracute infection: a sudden, overwhelming illness. The bird sits fluffed up and quiet, and death occurs within 2 – 3 days.
- Chronic infection: The bird fails to thrive for as long as 6 – 8 weeks. With treatment, some birds may recover; others will relapse and die. Some can live indefinitely with treatment, and the disease become transient and mild. 55
Part IV Pathogenicity and Etiology of Bacterial Disease
4.1 Classification Based on Pathogenicity
Pathogenicity is the capacity of an organism to cause disease. On this basis, bacteria which have been identified in a patient can be organized into three major groups:
- Primary pathogens. These are considered to be probable agents of disease (e.g., feces are tested and Salmonella spp. is identified as the cause of diarrheal disease).
- Opportunistic pathogens. These enter a host whose immune system has been compromised due to another disease. Bacterial infections can and do occur secondarily to other illnesses or pathogen infections. Viral infections, for example, cause a weakening of the immune system; this permits pathogenic bacteria to enter the body. 34
- Non-pathogens. Some bacteria are considered to be non-pathogenic because they rarely or never cause disease. Pathogenic bacteria constitute only a small proportion of bacterial species, and many non-pathogenic bacteria are beneficial to birds. However, it is possible for non-pathogenic bacteria to adapt and become harmful due to the effects of other therapies on resistance mechanisms. In fact, some bacteria previously considered to be non-pathogens are now known to cause disease.” 35
4.2 How Bacteria are Able to Cause Infection:
- Some bacterial species are extremely virulent and are able to attack a strong, healthy system.
- The bird encounters overwhelming or large-dose exposure to opportunistic bacteria.
Opportunistic bacteria are able to enter the system because of reduced immune response. This occurs during times of stress, poor nutrition, or concurrent disease conditions. Birds experience a great deal of stress some or even all the time. 19

Image 23: Fecal gram stain from a normal psittacine bird. (Image courtesy G. Kaufman) 31

Image 24: How sepsis takes over the body systems (image courtesy Dr. Warraich Health Channel) https://www.youtube.com/watch?v=qinhrQDtc_I&ab_channel=Dr.WarraichHealthChannel
Septicemia (sepsis or blood poisoning) is a systemic disease which results when pathogenic microorganisms and their toxins enter and remain in the blood. The signs seen by the clinician are a combination of those seen with toxemia and hyperthermia: fever and mucosal and conjunctival petechiation found in the joints, eyes, meninges (membranes around the brain and spinal cord), and heart valves. (Petechiae are minute reddish or purplish spots containing blood that appear in the skin or mucous membrane as a result of localized hemorrhage). Proof is by positive blood culture or smear.8
Sepsis, a life-threatening illness, is brought about by the presence of numerous pathological bacteria in the blood which cause the body to respond in organ dysfunction. 35
Image 25. Infection from bite wounds which can let to septicemia. Treatment needs to be aggressive (image courtesy N. Forbes). 23
4.4 Sources of Infection and Prevention
4.4.1 Bite Wounds from Cats and Other Animals
Bite wounds very often lead to a fatal septicemia if not treated aggressively. The patient should be evaluated for its overall condition and treated appropriately for blood loss or hypotension. The extent of wounds should be evaluated. If the patient’s condition allows, wounds should be thoroughly flushed and fractures stabilized. Aggressive antibiotics should be started early in the treatment. Piperacillin or cefotaxime combined with amikacin or tobramycin are a good choice and should be continued for up to 14 days. If septicemia is suspected, treatment for septic shock should be instituted, i.e., intravenous fluids, rapidly acting steroids, and intravenous bactericidal antibiotics.23
Image 26. Biliverdinuria and polyuria (excessive urination) in a cockatoo with bacterial septicemia and hepatitis (image courtesy Harrison and Ritchie: Making Distinctions in the Physical Exam, Section 2, Patient Evaluation in: Avian Medicine: Principles and Application, figure 8.41, p. 174, 1994
These are emergency cases which usually require that medications be delivered by parenteral means (other than by mouth) since the bird is unable to swallow them. “Treatment consists of administration of broad-spectrum antibiotics, parenteral fluid therapy, and corticosteroid administration to prevent endotoxic shock due to degenerating gram-negative bacteria.” 22
Pasteurella bacteria have been reported as possible septicemic agents in birds attacked by pet cats or rats. 30
4.4.1.1 Bartonellosis or Cat Scratch Disease
“Cat-Scratch Fever” is caused by a Gram-negative bacteria known as Bartonella henselae. It is spread through cat scratches and bites. The saliva penetrates the broken skin or mucosal areas such as the nose, mouth, and eyes. Licking by the cat will also transmit this disease. The wound is a puncture wound and it inoculates the bacteria into the skin, and because of the feathers, the owner doesn’t see it, then a few days later the bird is dead. 37
Cats use this toxic bacteria to kill in the wild; the instinct to attack, scratch, bite and claw are built into them. Infants, children, and adults can contract this disease from cats, even young ones. 37
The symptoms include:
- Blisters or papules at the site of the scratch/bite
- Fever, headache, sore muscles, poor appetite
- Heart, eye, brain, intestinal, and skin ailments
- Hyperplasic or swollen lymph nodes, particularly in the armpits and groin
- Malaise
- An enlarged spleen
- Fever, headache, fatigue, muscle soreness and poor appetite.
The diagnosis is often difficult to attain unless the parent is aware of the cat scratch/bite. A biopsy is required to establish a definitive diagnosis. Antibiotics such as Azithromycin are required to destroy the bacteria. Some pathogens are resistant to antibiotics, and this is becoming a serious problem. Most people recover in just a few weeks. In about 5-15% of cases, other, more serious conditions may develop, including heart, eye, brain, intestinal, and skin afflictions. 37
There has been some question about the incidence and potential for toxoplasmosis infection in birds, particularly in pet birds. For the most part, the possibility of pet birds kept in an indoor, hygienic, safe environment is low; however, there are some ways in which even these birds might contract the disease if cats are a part of the household. Many people now keep chickens and other poultry, and these birds are at risk of contracting Toxoplasmosis gonii infection as well. 37

Image 27. A new study reveals that the Toxoplasma gondii parasite acts through the IRE1 protein to cause infected cells to migrate through the body, spreading the parasite (image courtesy Drug Target Review). https://www.drugtargetreview.com/news/65528/toxoplasma-gondii-hijacks-host-stress-mechanisms-to-spread-through-the-body/
4.4.1.3 Toxoplasmosis Symptoms
Toxoplasmosis is a zoonotic (can be transmitted from animals to humans), parasitic, protozoan disease. It is more common in aviaries and backyard poultry than commercial producers. It is characterized by disorders of the central nervous system, but it can also affect reproductive, musculoskeletal and visceral organs (internal organs of the chest and abdomen). Clinical signs include:
- Weight loss and inappetence
- Shrunken comb (in poultry)
- Drop in egg production, whitish diarrhea
- Incoordination and trembling
- Opisthotonos (severe spasm in which the back arches; head is back and tail is up)
- Torticollis or Star-gazing (twisting of the neck)
- Blindness. All chickens infected before eight weeks of age develop clinical signs. In older birds, infection can be asymptomatic (infected hosts show no symptoms) or latent (symptoms only develop under certain conditions). 37
4.4.2 The Growth of Bacteria in Foods
Fruits, vegetables and other soft, moist foods can spoil rapidly, promoting the growth of bacteria (particularly Pseudomonas spp. and E. coli) Clean water with no additives should be provided daily. Vitamins added to the water oxidize quickly (become inactive) and provide an excellent growth media for bacteria. 24 Owners are advised not to add vitamins to water as there can be a 100-fold increase in the bacterial count in 24 hours. Changing the water and rinsing the container will obviously decrease the bacterial load, but an active biofilm remains on the container walls unless it is disinfected or washed thoroughly.38 Pseudomonas leaves a biofilm which is easy to detect and can be extremely harmful. Others, like Staphylococcus aureus, are difficult to detect and can be deadly. 24, 38
Salted, pickled, or cured foods will spoil more slowly and are less likely to grow bacteria. Remember your temperature guidelines: Keep it hot or cold. Storage in the refrigerator doesn’t prevent spoilage; it merely slows it down. Porous surfaces promote bacterial growth since they retain moisture.38 Soft foods can become contaminated with high concentrations of bacteria in as little as two to four hours, depending on the food, room temperature, and how old the food is. Food and water containers that have been contaminated with fecal matter will also grow bacteria in a short time. Utensils, storage containers, and towels can all be reservoirs for microorganisms. Don’t keep cooked grains such as pasta for more than a day or two. Freezing smaller portions is a good idea.11 38
Gram-negative bacteria can contaminate seeds, seed mixes, unwashed fruits and vegetables, and even tap water. 44 These bacteria are usually associated with water, sand, grit, seed, old food, humid areas, dusty spots and wet cages. Bacterial infections also occur in birds that have a poor level of natural resistance or a damaged immune system. 34, 44.
4.4.3 The Home Environment
Bacterial infections are always related to the environment in which the bird is kept. They usually result from ingestion of the pathogen or contamination in the location. Extra care must be taken to prevent recurrence. From the results of the culture tests, the veterinarian is able to explain the origins of each infection and can advise the client on ways to prevent recurrence. 34
Air conditioners and ventilation systems may serve as foci for bacterial or fungal growth in an indoor facility. In a finch breeding facility, recurrent bacterial infections were traced to an air conditioner filter that supported the growth of Aeromonas sp. 14, 22

Image 28. Contaminated food and water dishes on the bottom of the cage; filthy perches, cage and environment; perfect conditions for bacterial overgrowth (image courtesy Carla Treece Jackson; used with permission).
4.4.4 The Cage Environment
Food and water containers should be positioned away from perches or nest box openings to reduce excrement contamination. In Image 24, the feeding alcove was placed directly under the nest box, resulting in continuous excrement contamination of the food and water. Note also that these birds were on an all-seed diet. The incidence of recurrent enteritis in the breeding adults and Gram-negative bacterial septicemia in the neonates was high in this breeding facility. 14, 22
4.4.5 The Sick Bird
Sick birds should not be left out of the cage unattended; they should be either in their cages or with the owner until they are fully recovered. If allowed to wander around the house and on the floor, they could easily pick up other pathogens. This will protect them from becoming reinfected by bacteria in the environment. They can also pass the illness on to other birds when they are free-roaming. Ill birds are more susceptible to secondary infections. Birds already ill have little cell membrane resistance. 34
4.4.6 The Pet Bird’s Owner and His Family
Pet birds are at significant risk of infection by contact with their owners’ mouths. Most owners are not aware of all the bacteria in their mouths, and most of the time busy veterinarians don’t mention it in the birds’ annual exams.
4.4.6.1 Bacteria Found in the Human Mouth: E. coli
Current research shows that there can be over 600 different bacterial species found in a healthy human’s mouth. The bacteria most commonly found which can cause disease in birds are:
1. Lactobacillus
2. Clostridium
3. Corynebacteria
4. Proteus
5. Prevotella
6. Haemosphilus
7. Pseudomonas
8. Staphylococcus
9. Streptococcus
10. E. coli
11. Enterococcus
12. Mycoplasma
13. Neisseria
14. Actinomyces 61
Of all the bacteria found in the human mouth, E. coli is the most dangerous. It can be responsible for causing infections in psittacine birds, and it can even penetrate through the pores in egg shells, resulting in dead-in-shell embryos or death of recently hatched chicks. E. coli is identified as one of the most common causes of infection of the oviduct and reproductive tract in parrots.61
Because of the dangers present in the human mouth, it is crucial that everyone who handles the bird be made aware that kissing the bird on the beak and allowing the bird to kiss and tongue the human’s mouth allows transmission of bacteria to the bird’s mouth, thus providing entry of dangerous bacteria to the bird’s respiratory and gastrointestinal systems. The author has seen multiple videos and images of small birds being allowed to pick the teeth of a human. This practice invites serious bacterial infections in their avian companions. 61
“E. coli is a very common bacterial organism, found in human mouths at least 25% of the time, and it is also found in dog and cat feces, manure used to fertilize produce and flowers, and in the gastrointestinal tract of many animals we interact with on a daily basis. E. coli has the ability to proliferate uncontrollably outside of its normal home territory of the GI tract. But some strains of E. coli can also cause gastrointestinal disease and diarrhea, often dangerous and potentially fatal, if not identified and treated in time.” 61 It is diagnosed through cultures, lab tests, and DNA PCR. Blood chemistry tests and complete blood counts will help determine if this bacterium is present and causing the infection. Since this bacterium can survive in dried droppings and dander for a long time, constant cleaning and disinfecting of the environment is mandatory 61
4.4.7 T. gondii Parasitic Infection
Although this is not a bacterium, it is worth mentioning here as it is a danger to birds and humans. And since it’s a parasite, and can do considerable damage to the skin, bacterial infections can begin to form from the wounds on the bird’s tissues.
“Toxoplasma gondii (T. gondii) is a single-celled parasitic organism that can infect most animals and birds. Because it reproduces only in cats, wild and domestic felines are the parasite’s ultimate host. 11
“The only known definitive hosts for Toxoplasma gondii are domestic cats and their relatives. Unsporulated oocysts (eggs) are shed in the cat’s feces. Although oocysts are usually only shed for 1-2 weeks, large numbers may be shed during that time. Oocysts take 1-5 days to sporulate in the environment and become infective. Intermediate hosts in nature (including birds and rodents) become infected after ingesting soil, water or plant material contaminated with oocysts Cat litter boxes are the primary source of the infection in homes. 11
When a person becomes infected with T. gondii, the parasite forms cysts that can affect almost any part of the body — often the brain and muscles, including the heart. If a person is generally healthy, his immune system keeps the parasites in check. They remain in the body in an inactive state, providing the person with lifelong immunity so that he can’t become infected with the parasite again. But if his resistance is weakened by illness or certain medications, the infection can be reactivated, leading to serious complications. Women who are pregnant should have another person handle all cat droppings. 11
Although an adult can’t “catch” toxoplasmosis from an infected child or another adult, he can become infected if he comes into contact with cat feces that contain the parasite. The person may accidentally ingest the parasites if he touches his mouth after gardening, cleaning a litter box, or touching anything that has come in contact with infected cat feces. Cats who hunt or who are fed raw meat are most likely to harbor T. gondii.” Anti-parasitic drugs are used to counteract the disease. 11
4.5 Disinfection: The Key to Preventing Disease
Clean all food and water dishes daily; this is particularly important if the bird has an infection, but it should be part of the daily cage-cleaning routine. Lysol and dilute bleach are very good at disinfecting. It’s best not to clean with these solutions; just use them as disinfectants after cleaning with detergent or soap and water. The Lysol and bleach have instructions for how long the liquid is supposed to remain on a surface. And proper dilution is key—straight bleach is very corrosive. When cleaning bird-occupied surfaces, use 1 part bleach to 10 parts water. Disinfectants and cleaning products all work by different methods, although bleach is pretty much toxic to everything. The owner should wear gloves; inexpensive neoprene gloves are available at hardware stores. 38
Clean and disinfect perches often. Keep the birds away from the cages when you are cleaning them until the cages are completely dry.
Part V: Bacterial Pathogens Commonly Found in Companion Birds
Explanation of Gram’s stains and Gram positive and negative bacteria and other tests will be found in Part VI
5.1 Commonly Found Gram-positive Bacteria
- Staphylococcus, including Staphylococcus epidermidis.
- Streptococcus and Streptococcus intermedius
- Clostridium
- Enterococcus
- Mycoplasma spp (has been implicated in chronic sinusitis and often found in cockatiels)
- Lactobacillus
- Corynebacterium. 26, 34
5.2 Commonly Found Gram-Negative Bacteria
- Klebsiella
- Aeromonas
- Enterobacter
- Proteus
- Citrobacter
- Pseudomonas
- Campylobacter
- Escherichia coli,
- Pasteurella spp
- Mycobacterium and Chlamydia
- Salmonella spp.18, 23
Image 29. Fig 39.24 | A canary with Mycoplasma conjunctivitis CAM: Bacterial Diseases 895-897 Bacterial disease in Passeriformes (songbirds, canaries, finches)
5.3 The Most Dangerous Gram-Positive Bacteria: Staphylococcus and Streptococcus
Staphylococcus (plural staphylococci) and streptococcus (plural streptococci) infections are commonly found in many pet birds and often discussed together. They both will produce severe illnesses that will lead to death. These bacteria are responsible for a wide variety of symptoms, including
- dermatitis,
- pododermatitis (bumblefoot),
- conjunctivitis (red, inflamed eyes),
- sinusitis,
- arthritis, and
- pneumonia
Initial testing is usually with Gram’s stains and cytology, and confirmation of the disease is provided with culture-and-sensitivity testing. 28 Staphylococci, streptococci (especially hemolytic strains), and Bacillus spp are thought to be responsible for several dermatologic conditions in psittacine birds. 26

Image 30. S. aureus with pyloderma grown in a culture (image courtesy Galabin Mladinov гълъбин младенов; used with permission)

Image 31. Sinus infection in a cockatiel due to a bacterial infection, probably S. aureus. A scab has formed over the eye and it is likely the orbit has collapsed, rendering the bird blind in that eye (image courtesy Bob Doneley; used with permission). 18
5.3.1 Staphylococcus aureus and MRSA
Staphylococcus is a genus of spherical, gram-positive bacteria which occur in grape-like clusters. They are a natural part of skin flora in most mammals and birds, and they normally colonize the upper respiratory, alimentary, and urogenital tracts. They are also the most common cause in pus-forming (pruritic) skin infections. S. aureus, commonly found in the nares, and S. epidermidis, found in both the nares and on the skin, have the greatest pathogenic potential. 45
Staphylococci are often isolated from lesions of pododermatitis in many avian species. Methicillin-resistant S. aureus (MRSA), previously thought of as rare, is becoming increasingly documented in birds. This bacterium is found in dust, poor seed, contaminated air conditioning, and is carried by mice. It is exacerbated by stress. 26
For a comparison of S. aureus and MRSA, please see Appendix A, p. 75

Image 32. Bumblefoot Caused by S. aureus usually in birds. A pyogranulomatous, chronic infection of subcutaneous tissue on feet. S. aureus is usually introduced via skin lesion on foot (image courtesy Study Blue, Gram positive Bacteria Flashcards | Chegg.com). https://www.chegg.com/flashcards/staphylococcus-c38dfd0f-1879-4025-bc55-d3167c8935da/deck
5.3.1.1 Antimicrobial Resistance of S. aureus
Staphylococcus aureus is resistant to most antibiotics.26 “S. Aureus and Streptococcus have acquired resistance through genetic mechanisms. Many strains of S. aureus are resistant to all clinically useful drugs.” 45
Staphylococcus infections generally result in very pruritic (red, itching and pus-filled), often erythematous (red blood cell) infections of the skin. Skin biopsy—including that of feather follicles—and cultures are required to diagnose the illness. 18

Image 33. Dermatitis in a cockatoo due to staphylococcal infection following a dog ‘mouthing’ the bird (image Courtesy B. Doneley; used with permission).18
5.3.1.2 Case Study Involving S. aureus
A 2-year-old female Congo African Grey parrot (Psittacus erithacus erithacus) was evaluated for long-standing self-trauma of the feathers and skin of the tail base. All tail feathers and tail coverts were missing, the skin of the tail base was thickened and ulcerated, and the uropygial gland was swollen. There was increased white blood cell count, and x-rays showed shortened caudal vertebrae and pygostyle. Test results of affected areas “revealed ulcerative bacterial dermatitis positive for methicillin-resistant Staphylococcus aureus (MRSA).” 9
The bird was treated with multiple medications, topical gel, and hydrotherapy for a month, and there was some tail feather regrowth; however, even though the bacterial infection was resolved, the bird continued to traumatize the area for the next two years. 9

Image 34. Staphylococcus aureus (image courtesy Food Science Avenue). https://www.foodscience-avenue.com/2018/01/staphylococcus-aureus-toxin.html
Streptococcus (plural Streptococci), is a disease-causing, Gram-positive bacteria frequently seen in birds. It is found everywhere in the environment, mainly in the dust and air. Many species have been isolated from birds, and they are considered part of the normal bacteria found on the skin and the lining of the digestive, respiratory, and reproductive tracts. 19
The immune competency of the bird will determine whether or not the bacterial growth increases sufficiently to become a disease agent. 55
Some species of Streptococcus are zoonotic. It can be found in humans’ mouths, sinuses, and eyes. 19

Image 35. Streptococcus pyogenes (image courtesy WikiMili).
Streptococcal infection in poultry – WikiMili, The Best Wikipedia Reader
Group A streptococcal infection – WikiMili, The Best Wikipedia Reader
5.3.2.1 Streptococcus Bacterial Invasion
The streptococcus organism invades the body of a susceptible bird and spreads, first invading the bloodstream from the intestines or skin and then traveling to the other areas of the body. It usually localizes in one specific area initially and then continues to spread. Some of the possible entry areas of the body are:
- The respiratory system, leading to red, watery eyes, nasal discharge, and difficulty breathing.
- The liver, with green diarrhea (biliverdinuria) and weight loss.
- The heart, with long-term cardiac issues and chronic shortness of breath.
- The meninges of the brain, leading to poor coordination, loss of balance, or head tilt.
- The muscles, leading to bleeding and inflammation
- The joints, leading to redness and pain, especially in the wings and legs.
- The kidneys, with increased thirst and urination.
- The intestines, leading to diarrhea
- The abdominal cavity, leading to ascites (fluid buildup) and swelling in the abdomen.
- The reproductive system
- Young males might experience premature infertility.
- Hens may experience poor egg formation, leading to embryonic death and weakened chicks that die during or shortly after hatching.
The organism is found in birds’ droppings and can contaminate the nest box and infect the healing navel of recent hatchlings.” 55
5.3.2.2 Diagnosis and Treatment of Streptococcal Bacteria
Diagnosis is based on the patient’s history and clinical signs. It depends on the isolation of the bacteria from lesions and cytology findings of streptococcus bacteria in blood films or impression smears of affected tissues. 40

Image 36. Streptococci and Enterococci bacteria. Oval cells are arranged in chains end-to-end (image courtesy Medical Microbiology).
Sherris Medical Microbiology, 6e | AccessMedicine | McGraw Hill Medical (mhmedical.com)
Healthy birds living in well-kept environments will be able to resist the disease, and those who do become ill will be able to recover with medication. In an aviary or breeding situation, once the streptococcal disease is diagnosed, the owner must identify and correct the cause of the disease outbreak; otherwise, the medication will not be successful. 55
S. aureus will respond to antibiotic treatment. Identification of the organism through culture and sensitivity testing enables the veterinarian to prescribe the most effective antibiotic for that particular strain. Studies show that doxycycline has become the drug-of-choice for most practitioners. It is as effective as synthetic penicillins and more economical. According to Walter, 80% of organisms are controlled by the antibiotics ampicillin (a synthetic penicillin) and doxycycline. 55

Image 37. Streptococcal infection in the patagium of the wing of the author’s bird. The bird died from this infection (image courtesy J. Miesle)
5.3.2.3 Preventing the Spread of a Streptococcal infection.
“Streptococcal infections will spread slowly through the flock, resulting in the deaths of some of the birds. Once the disease is confirmed, follow the recommendations below:
- Separate ill birds and treat them in a hospital cage environment (heat, fed and medicated by crop tube, etc.) or euthanize them.
- Keep the aviary clean and disinfected at all times.
- Identify and correct any trigger factors, such as overcrowding, poor diet, poor hygiene, inadequate parasite control, cold or damp conditions.
- Start healthy birds on probiotics. If further birds continue to become unwell while on the probiotic treatment, then treat the entire flock with an antibiotic such as doxycycline.” 55. “Probiotics will help to minimize the streptococcal invasion during stressful times when normal intestinal bacteria are disrupted; in addition, they may prevent transmission of the infection to other birds.” 55

Image 38. A rescued cockatiel taken in by the author. This bird was suffering with a severe sinus infection involving S. aureus.
To view the case study of this cockatiel, please see Appendix B, p. 75
E. faecalis was known as Streptococcus faecalis until 1984 since it was previously categorized by scientists as a bacteria that forms part of the Streptococcus genus. Passerines, or songbirds, such as finches and canaries, are often found with Enterococcus faecalis (formerly Streptococcus bovis) which resides in the alimentary tract. “Birds with this bacteria will present with chronic tracheitis, pneumonia, and air sacculitis, increased respiratory sounds, voice changes, and dyspnea (labored breathing).” 28
Canaries are especially sensitive. Although antibiotics will provide improvement in the clinical signs, many birds never heal completely. 20

Image 39. Enterococcus faecalis (image courtesy Px Pixels). https://pixels.com/featured/9-enterococcus-faecalis-dennis-kunkel-microscopyscience-photo-library.html
5.5 Mycobacterium Avium, or Avian Tuberculosis
Mycobacteria are straight or slightly curved, non-motile, Gram-positive rods. Most birds, including psittacines, are susceptible to M. avium. It is mostly found in high-density populations, such as zoos, breeding facilities, and larger collections. 3 “Mycobacteriosis is an infectious, systemic disease which is chronic and debilitating.” 15
In the past, antemortem (before death) diagnosis had been challenging, so clinicians had only tests and history to diagnose it. Today, however, clinicians use molecular diagnostic testing since it will afford a definitive diagnosis. 15 For some birds, diagnosis will not be obtained until the postmortem is performed. 49 “Mycobacteria infection leads to a chronic wasting disease. Granulomatous, inflamed lesions on the skin develop that are easily confused with tumor masses.” 21
It may be difficult to determine if birds in large collections are infected. The clinician and owner will need to work together to assess the husbandry and sanitation levels in the aviary. It is important to isolate the birds who have the disease or are at risk of contracting this disease. Their weights should be monitored, and CBCs and fecal, acid-fast stains or PCR testing should be performed. 26

Image 40. Cutaneous form of avian tuberculosis in collared dove (image courtesy Datashare).

Image 41. Avian tuberculosis in a woodpigeon. Large, cream, raised nodules throughout liver (image courtesy Datashare).
5.5.1 Vulnerability
Several species of birds are highly susceptible to the disease: gray-cheeked and canary-winged parakeets (Brotogeris pyrrhoptera), Amazon parrots, pionus, finches and canaries, and some species of Forpus parrots (parrotlets). This disease is endemic in these populations, making the birds predisposed to acquiring it; for them it can be quite debilitating. Softbills and passerines are highly susceptible to mycobacterial infections as well. 21, 26, 49
Image 42. Avian mycobacteriosis (image courtesy N. Forbes). 23

Image 43, Mycobacteriosis in the lung (image courtesy VMD labs; used with permission). http://www.vmdlabs.com/ada-Mbac.html

Image 44. Mycobacteriosis in the duodenum (image courtesy VMD labs; used with permission). http://www.vmdlabs.com/ada-Mbac.html
Mycobacteriosis is one of the most common diseases of various species of birds including domestic poultry, pet and exotic birds such as psittacines and canaries, and free-living and captive wild birds. The disease in birds is generally caused by Mycobacterium avium, but more than 10 other species of mycobacteria have been known to infect birds. These include M genavense, M. tuberculosis, M. bovis, M. gordonae, M. nonchromogenicum, M. fortuitum subsp fortuitum, M. avium subsp hominissuis, M. peregrinum, M. intermedium, M. celatum, M. intracellulare, M. avium subsp paratuberculosis, M. africanum, and M. simiae.
5.5.2 Transmission
M. avium-infected fecal matter, once aerosolized, will be put into the air in large amounts. The infected birds will shed this, and it is then transmitted by ingestion and inhalation. 3
The organism enters the body through the oral, respiratory, and dermal routes. “If the organism enters by ingestion, in will invade the intestinal tract, causing bacteremia, and spread to the liver and other organs.” 15 Ingestion of the bacteria through contaminated food or water and fecal matter is the most common mode of transmission. 15
The incubation period for birds is weeks-to-years. The bird will develop pulmonary lesions if the bacterium is inhaled, and skin disease may also develop. It is possible that the bacterium is spread vertically, from hen to egg, but that mode of transmission is not common. 3
5.5.3 Symptoms
Since Mycobacteriosis is difficult to diagnose in its early stages, it should be considered as part of the differential diagnoses when these symptoms are observed:
- Weight loss in spite of good appetite
- Emaciation and muscle wasting
- Loss of subcutaneous and intracoelomic (internal) fat
- Poor-quality integument and skin
- Diarrhea and green urine
- Dyspnea
- Seizures
- Lesions in the lungs and air sacs from inhalation
- Paralysis and lameness
- Depression
- Increased thirst and urination
- Abdominal distention
- Respiratory distress
- Decreased egg production. 3, 15
“Strong indicators of the disease are:
- Subcutaneous granulomas (small, inflamed growths under the skin)
- Organomegaly (enlarged organs)
- A profound leukocytosis (elevated number inflamed white blood cells)
- The cytologic presence of acid-fast bacteria
- Masses and ulcers with enlargement of joints, especially for those with negative results for fungal and aerobic/anaerobic bacteriologic cultures.” 15
5.5.4 Testing
Several tests may be performed to determine the bacterium. “PCR assays will detect the actual disease-causing organism, and ELISA assays will detect specific antibodies for M. avium. PCR assays are considered to be the fastest, most sensitive method for detecting M. avium, while ELISA assays help determine exposure to M. avium.”3 Molecular methods are highly sensitive and specific for confirming the disease in a short amount of time. 15
“Endoscopy allows for direct visualization of infiltrative lesions in the abdominal cavity and respiratory tract.”3,15 With it, clinicians are able to:
- “Identify lesions on the serosal surface of the liver, spleen, intestine, lung, and air sacs.
- Visualize granulomas as white, yellow, or tan, round masses which are soft and easily biopsied. Visualize enlargement of the liver, kidneys, and spleen.
- Take samples of abnormal tissues or granulomas to confirm the diagnosis of mycobacteriosis.
- Remove samples of lesions for cytologic or histopathologic examination, acid-resistant staining, culture, and molecular tests. Examination of the liver is crucial when diagnosing avian mycobacteriosis.” 15
The antibiotic used is determined by the bird’s age, species, and bacterium found. Azithromycin is the drug of choice. It can take six to twelve months to resolve the disease, and relapses are common. Owner commitment is essential since the bird will need daily dosing. Keeping the flock size low and the stress levels reduced will minimize the impact on the collection. Young birds still hand-feeding respond well with oral medications, whereas adult birds respond better to injectable therapy. Combinations of antibiotics (typically three) are recommended because many mycobacterial organisms develop antibiotic resistance. Birds with advanced disease and granuloma formation have a poor prognosis. 26, 49
5.5.6 Prevention
Preventing M. avium is best done by minimizing stress and overcrowding and by providing proper ventilation and nutrition. M. avium outbreak in zoos, bird gardens, and private aviaries can be especially difficult to eradicate. New additions to the aviary should be quarantined for a minimum of 1-2 months. New additions to the flock should be tested to prevent outbreaks. 3
Although rare, sudden death might be an indication of mycobacteriosis. Generally, though, “acute death from mycobacteriosis is unusual.”15 Biopsies of the liver, GI tract, spleen, and lungs will diagnose the disease at necropsy 3
Pathology results include:
- “Emaciation
- Absence of subcutaneous and internal fat
- Severe atrophy of the pectoral muscles
- Hepatomegaly and splenomegaly (enlarged liver and spleen)
- White or yellowish nodules in the lungs, spleen, intestine, air sac, bone marrow, and more rarely, the heart, gonads, central nervous system, skin, and joints.
Hematologic (blood) changes reflecting chronic inflammation and anemia. 15
5.6 Yersinia pseudotuberculosis
Yersinia pseudotuberculosis is a common cause of outbreaks of acute illness and mortality, usually in aviary parakeets. It is transmitted via feces from infected rodents and wild birds. The majority of affected birds die within a few days, having shown signs of pneumonia, enteritis with wet diarrheic droppings, and general ill health. At post-mortem examination, the most acute cases have an enlarged, patchily discolored liver, and more chronic cases have miliary white spots throughout the liver, kidneys and spleen. 53
In a living bird, confirmation by bacteriology is needed, and antibiotic treatment is required. The drinking water must be kept uncontaminated, and the water should contain either the appropriate antibiotic or a disinfectant, such as 5–6 mg/L of free iodine or chlorhexidine. Prompt treatment will limit, but not completely prevent, deaths in the affected birds. The organ damage in some individuals will cause their deaths even in the absence of the organism. 53
Image 45. Miliary granulomas as seen on this canary’s dark and swollen spleen are indicative of Yersinia pseudotuberculosis (image courtesy Clinical Avian Medicine, Chapter 39, p. 897 figure 39.26
Canaries and finches, particularly in Europe in the winter, may be found with the infection. Signs include ruffled feathers, debilitation, and high mortality. At necropsy, a dark, swollen, congested liver and spleen with small, yellow, focal bacterial granulomata are often found. Diagnosis is confirmed after culturing the microorganisms. Amoxicillin via drinking water is the antibiotic of choice. Soft foods are recommended. 53
Mynahs are very susceptible to yersiniosis, and mortality can be high due to a peracute pneumonia. Post-mortem examination demonstrates hepatomegaly, sometimes with small white foci, splenomegaly, and an acute-to-peracute pneumonia. In Europe, a formalin vaccine is available that appears to be clinically effective in reducing the prevalence of infections. 53

Image 46. E. coli bacteria (image courtesy S. Weir) 56
Escherichia coli exists in small numbers in the intestinal tracts of many species of birds, and only if the numbers rise is there a problem. Symptoms vary from species to species. E. coli infections are classified as primary or secondary: A primary infection causes disease by itself, and a secondary infection has an underlying cause. “Most infections are secondary to such stressors as a heavy molt, coccidia, adenovirus, canker, intestinal worms, crowding, stressful home conditions, and poor nutrition.” 56
Contaminated food, fluctuating temperatures, drafts, stress, wet areas, fungal infection, and dirty cages are some of the most common causes. 26, 34
5.7.1 E. coli Diagnosis and Treatment
Diagnosis of E. coli infection is based on the symptoms. These are:
- Enteritis and necrotic enteritis
- Loose, green droppings (biliverdinuria)
- Crop stasis
- Vomiting and weight loss
- Sudden death due to septicemia
E. coli, like salmonella, may result in joint infections which present with lameness, swelling, or a drooped wing. Immediate attention to these signs is necessary to prevent further joint damage from occurring. 55
Gram-negative bacteria are usually associated with disease in birds; however, the number of bacteria in the intestines differs among species, and some are not pathogenic. Neotropical birds, such as amazons, “may have little to no E. coli in their systems, while some species, such as cockatoos, lories, and eclectus parrots, may have as much as one-fourth of their total flora comprised of E. coli.” 35 As long as the number of bacteria is low, most clinicians believe there is no need for treatment if the bird is not showing clinical signs, but if the bacteria are found in chicks and juveniles, the clinician should perform more tests and begin treatment. 49 
Image 47. Dropping from a bird with hemorrhagic enteritis, cultured E. coli. Bleeding from an infection/inflammation in the lower intestinal tract (image courtesy M. McMillan: In: Diseases of Cage and Aviary Birds. Ed. Margaret Petrak.1982)
Some strains of E. coli are quite resistant to antibiotics. Commonly used medications are azithromycin, Baytril, Cipro, or Bactrim. These are not to be used on birds that are breeding. The underlying cause of E. coli must be found and treated or the bacteria will return. 56
Campylobacter is a genus of bacteria of the family Spirillaceae. It is a spirally curved, motile, Gram-negative, rod-shaped bacterium which is pathogenic in domestic animals and humans. Wild and domestic birds are considered major reservoirs of Campylobacter bacteria. It has been found in 35% of migratory birds, 50% of town-dwelling pigeons, and 20%-70% of gulls. It is most commonly found in poultry; therefore, eating undercooked or raw chicken will cause illness in humans and animals.12, 40

Image 48. This shows the curved shape of Campylobacter species (arrow A showing curved gram negative bacteria, arrow B showing white blood cell) stained by gram stain using 0.3% as counter stain. Original magnification X100 (image courtesy Jeremiah Seni, Research Gate). https://www.researchgate.net/publication/271214444_Evaluation_of_detection_methods_for_Campylobacter_infections_among_under-fives_in_Mwanza_City_Tanzania/figures?lo=1
. 
Image 49. Campylobacter jejuni (image courtesy Go Pets America). http://www.gopetsamerica.com/bio/bacteria/campylobacter.aspx
The species most often seen in enteric disease in avian species is C. jejuni. Infected birds may be asymptomatic or show the following signs:
- Anorexia
- Somnolence
- Diarrhea
- Emaciation 43
5.8.1 Transmission and Diagnosis
This bacterium is fatal in very young birds. Transmission is by direct fecal or aerosol contact, contaminated fomites (things which other birds have touched), or infected vectors (an organism such as an insect that transfers the bacteria from one animal to another). Diagnosis is made by microscopic examination of the droppings using Gram’s stains. 31
5.9 Clostridium
Clostridia are anaerobic, gram positive, spore-forming bacteria. Members of this genus resemble large, straight, or slightly curved rods with rounded ends. Clostridial organisms are common secondary invaders of damaged cloacal tissue in birds with cloacal prolapse or  papillomatosis. Different species of clostridia can cause specific disease syndromes. 26
papillomatosis. Different species of clostridia can cause specific disease syndromes. 26
Image 50. Clostridium perfringens (image courtesy University of Arizona, College of Agriculture). https://cals.arizona.edu/pubs/general/resrpt1998/clostridium.html

Image 51. Gram positive clostridium botulinum, or bacillus botulinus (image courtesy Pixnio.com) https://pixnio.com/science/microscopy-images/botulism-clostridium-botulinum/gram-positive-clostridium-botulinum-formerly-known-as-bacillus-botulinus
Image 52. Clostridium in a 7-year-old Moluccan cockatoo presented for smelly stool. In the bacteria field there were 90% gram-positive rods, 10% gram-positive cocci, and 30 Clostridium sp. organisms (image courtesy Merck Veterinary Manual). http://www.merckvetmanual.com/exotic-and-laboratory-animals/pet-birds/bacterial-diseases-of-pet-birds#v4631674

Image 53. Microscopic illustration of rod-shaped bacteria such as Clostridium (image courtesy 123rf) https://www.123rf.com
Clostridium perfringens is the species most often seen in psittacine birds. C. perfringens secretes strong exotoxins that can cause necrosis (cell death) of the surrounding tissue, including muscular tissue. The bacteria “produces gas that leads to bubbly deformations of the infected tissue.” C. perfringens will destroy intestinal tissue, and the enterotoxins lead to severe diarrhea. 2

Image 54. Gas in a bird’s droppings is never normal. Here, diarrhea is caused by gas-producing bacteria (image courtesy Avian Biotech). 2
The clostridia toxins in the small intestines produce these symptoms:
- Decreased appetite and rapid weight loss
- Loss of body condition
- Lethargy
- Blood-stained or undigested food. 2
The toxin and its effects may continue to be in the bird’s system for quite some time, even after the infection has been resolved. 2

Image 55. Clostridial Enteritis (image courtesy Todd Driggers; used with permission).
Yellow blotches: slide artifacts; Purple blotches: degenerating white blood cells; Blue rods: non-sporulated clostridial rods; oval green blotches with black centers: red blood cells
Transmission is by ingestion and wound infection from spores found on contaminated surfaces. The spores may also be inhaled or be on contaminated feed, water, fecal material, air, soil, and nesting material. 2 Infection may be avoided by:
- Minimizing stress and overcrowding
- Providing proper ventilation
- Preventing malnutrition with a proper diet. 2
Storing food properly in containers will prevent bacterial growth. Corn and grain products, and even pellets or extruded food, may be contaminated by bacterial spores if conditions are favorable. It is wise to freeze all food coming into the house until it is used. 2
5.9.3 Diagnosis and Treatment
Gram’s-stained smears and anaerobic cultures are used to identify clostridial organisms. Samples from affected tissue are used, “including the greenish-brown focal areas of necrosis in the liver. Large, gram-positive cells are almost certain to be clostridia, especially if spores are seen.” 26
Antitoxins and antibiotics, such as Guanidine, zinc bacitracin, penicillin, and tetracyclines are used to treat this bacterium. 2

Image 56: Salmonella bacteria (image courtesy Avian Biotech). 2

Image 57. Salmonella growing on XLD agar (image courtesy Nathan Reading on Flickr [CC-BY-2.0], via Wikimedia Commons.https://www.yourgenome.org/facts/what-is-salmonella
Salmonella species are gram negative, aerobic, rod-shaped, zoonotic bacteria that can infect people, birds, reptiles, and other animals. 4
Salmonella typhimurium is the organism most frequently seen in psittacines. Clinical signs are severe illness followed by acute death from septicemia. Rodent feces are a source of contamination in the aviary, and rodents will contaminate food supplies and nest boxes; they will carry contaminants from their own nests to the aviary. 49
FREE Training to Stop Your Bird's Biting
Get FREE access to Beak School – the only system designed to train your bird. Stop behavioral problems like biting, screaming, feather plucking.
Get the Free Training5.10.1 Infection and Transmission
Infection from S. typhimurium can result in high mortality of young birds. Transmission among birds is primarily through the air. “The organism remains stable outside the host body and dries as a dusty substance.” 4 This contaminated dust becomes airborne and enters other birds’ respiratory systems by direct contact of aerosolized fecal matter or feather dust. Affected birds may become symptomatic or be carriers. Transmission is also by ingestion of contaminated food or water, or through shedding the organism in nasal and ocular secretions. Degree of infection depends on the bacteria levels, their serotype, and the age, species, and condition of the host. Birds may have peracute, acute, chronic, or subclinical infection. 21
The susceptibility of the bird and number of spores in the environment determine whether or not the bird will become infected. The young may become infected through regurgitation from the hen’s crop during feeding.21
5.10.2 Clinical Signs and Susceptibility
- Depression
- Lethargy
- Anorexia, diarrhea, and weight loss
- Conjunctivitis
- Pasty vents
- Lameness
- Abscess formation
- Convulsions
- Poor hatching or excessive fledgling mortality
- Dehydration and crop stasis
- Meningitis
- Liver, kidney, spleen and heart damage and lesions
- Osteoarthritis
- Sudden death.
- Pneumonia and excessive mucus in the nose or throat with inflammation of the mucous membrane.
- Hemorrhagic enteritis 4, 21
Some avian species have specific clinical symptoms. Lories (Loriidae) suffer acute disease and high flock mortality. African Greys tend to develop chronic disease, and their symptoms are mucus discharge from the beak/nasal area, arthritis, excessive thirst, and dermatitis. “Droppings are colored a sulphur yellowish green which is very much a diagnostic sign for this microorganism.” 4
5.10.3 Transmission and Diagnosis
Transmission from hen to egg (vertically) is possible. If this occurs, chicks will hatch and spread salmonella by direct contact with other birds. If the bacteria level is high, the embryo will die. “The disease has a greater chance of spreading in overcrowded conditions, stale air environments, nest-boxes, and brooders. Pet shops, bird marts, and quarantine stations are also high-risk areas.” 2
In the past, fecal and affected organ culture-and-sensitivity testing have been used to diagnose and treat salmonella. Antemortem diagnosis by fecal cultures is difficult because the bacteria is shed intermittently. 21 Today, these assays have been replaced by PCR and sequence assays which are more reliable and identify the strains more precisely.4 Even with prolonged treatment (3–8 weeks), the organism might not be eliminated. This disease is controlled only with “strict isolation, vector control, and appropriate disinfection.” 4, 21

Image 58. Salmonella typhimurium (image courtesy Pathogen Profile Dictionary). http://www.ppdictionary.com/bacteria/gnbac/typhimurium.htm
5.10.4 Prevention and Treatment
To prevent outbreaks of salmonella, it is important to keep the birds’ environment meticulously clean. Effective control of flies, rodents and other vermin is essential to eliminate and prevent salmonella outbreaks. Companion birds may be infected by humans who carry the bacteria. African greys, Amazons, cockatoos, and macaws are especially at risk. 4 Hanamycin, Gentamycin, and trimethoprem/sulfamethoxazole are used to treat this disease.
5.11 Chlamydiosis. (Ornithosis or Parrot Fever in Birds, Psittacosis in Humans)
Chlamydiosis is the most important zoonotic disease of psittacines. It is endemic to the U.S. and in the wild population.30 Macaws, cockatoos and Amazons are particularly vulnerable to this bacterium. It is also found in cockatiels, budgerigars, and parrots. 26, 33
Chlamydia psittaci is an obligate, intracellular bacterium that can infect all companion birds. The incubation period of C psittaci is from three days to several weeks. The organism can remain infectious in organic pus for about one month. 26 The severity of the disease in the bird depends on the virulence of the organism and the competency of the bird’s immune system. 30.
“Chlamydophyla depends on amino acids and the host’s cells for its energy supply. The bacterium targets epithelial cells of the mucus membranes of the respiratory system and digestive tract.” 46

Image 59. Chlamydia psittici in the air sacs (image courtesy Veterinary Molecular Diagnostic Labs; used with permission). http://www.vmdlabs.com/ada-Chlam.html
Diagnosis of C. psittaci is difficult, particularly if the bird is asymptomatic. History, clinical signs, radiographs, CBC’s, chemistry panels, and cloacal and choanal cultures have been used in the past, but now serology and PCR testing have proven more reliable. 26, 30
5.11.2 Transmission
For now, there is not a test to show if a previously infected bird is free of the disease. It is transmitted through aerosol inhalation and ingestion for the most part. 21 Birds may initially be asymptomatic, but stress can cause acute illness. These birds will infect other birds and humans by shedding the organism. Cockatiels are thought to be one of the most common asymptomatic carriers of C. psittaci. 30 Because it is a zoonotic disease, federal regulations require it to be reported. 26
Birds may be asymptomatic carriers, or they may have severe disease. Clinical signs may include:
- Chronic ocular, nasal, or conjunctival irritation and discharge
- Anorexia, dyspnea, dehydration and polyuria
- Depression
- Biliverdinuria (dark green stools and urine) (hepatitis)
- Hepatomegaly, splenomegaly (enlarged liver and spleen), or air sacculitis.
- Upper respiratory signs (conjunctivitis/sinusitis/rhinitis, often seen in cockatiels)
- Vomiting, lethargy, chronic diarrhea, weight loss
- CNS signs at late stages of the disease which include opisthotonos (arched back), tremors, and convulsive movements
- Leg paresis or paralysis
- Sickly, unthrifty bird with repeated episodes of illness.
- Poor feather coat 21, 26, 30, 33

Image 60. Chlamydia – Direct imprint from air sac with DifQuik stain showing an initial body (image courtesy G. Kaufman) 30

Image 61. This impression smear, made from the exudate of infected tissues, shows intracytoplasmic inclusions associated with Chlamydophila psittaci. Histopathology image from a turkey (image courtesy Cornell University). http://cidc.library.cornell.edu/vet_avian/images/Chlam-Adjusted/CHLAM-022A.jpg.infection. https://partnersah.vet.cornell.edu/content/chlam-022ajpg

Image 62. Chlamydia Psittici in a cockatiel (image courtesy Edgeworth Animal Medical Center). https://www.edgeworthanimalmedical.com.au/2017/05/05/avian-chlamydiosis-and-psittacosis/

Image 63. Photomicrograph of Chlamydophila inclusions in macrophages (arrow) in an Amazon parrot.. Giemsa Stain was used (image courtesy Brazilian Journal of Veterinary Pathology).
Doxycycline and azithromycin are the drugs of choice for Chlamydia infection. It is unknown exactly how long it takes to eliminate the organism from the body; therefore, it is recommended that the bird be treated for 45 days. 26

Image 64. Dropping from a cockatoo with psittacosis (image courtesy Cockatoo Info.) http://cockatoo-info.com/health/chlamydia-psittacosis/

Image 65. A Bourke parrot with conjunctivitis caused by Chlamydiosis (image courtesy Melbourne Bird Vet; used with permission). http://birdvetmelbourne.com/chlamydiosis/
Other drugs that have been used to treat Chlamydia in birds are:
- Tetracyclines. They are very effective but work only during the active dividing stage of the organism. For this reason, prolonged therapy for 45 days is required. Even after successful treatment, you can never guarantee a bird free of the organism.
- Chlortetracycline. Treatment through the drinking water is not acceptable.
- Fluoroquinolones are very effective against this organism. 30
For more information, see https://www.beautyofbirds.com/psittacosis.html
Bordetella is a gram-negative, aerobic, coccobacillus bacterium of the Bordetella genus. This rod-shaped bacterium is non-motile and non-spore-forming. B. avian causes the avian disease, bordetellosis, which is responsible for respiratory tract infections in turkeys and in wild and domesticated birds. 36 It is most commonly seen in birds between the age of 2-8 weeks. Turkeys are thought to be the natural host, however; the disease has also been seen in chickens and ducks. 60

Image 66. Bordetella avium in a cockatiel (image courtesy Veterinary Molecular Diagnostic Labs; used with permission). http://www.vmdlabs.com/ada-Bord.html
“B. avium colonizes the epithelium of the cockatiel’s tracheal mucosa. As the disease progresses, it will destroy this outer layer of tissue along the respiratory tract and produce toxins that can affect other groups of tissue in the body. It is not zoonotic to humans.” 60
As it damages the upper respiratory tract of the bird, it leads to secondary infections from E. coli or other bacteria, causing a more severe infection. If the bird is infected solely with B. avium, he may recover in 4-6 weeks with treatment. Without treatment, the disease will destroy the epithelial tissue in the trachea, causing the bird to die from suffocation. 27
Bordetella is highly contagious and easily transmitted by direct contact. It is doubtful that it is airborne because birds near an infected bird will not get the disease. 21 It can also be transmitted through contaminated drinking water, feed, bedding, housing, and litter and can remain infectious for 1–6 months in contaminated litter. 27

Image 67. Bordetella avian (image courtesy Look for Diagnosis). https://lookfordiagnosis.com/mesh_info.php?term=bordetella%20avium&lang=3
Signs appear suddenly and include:
- Sneezing and coughing, mouth breathing and dyspnea
- Foamy conjunctivitis around the medial canthus (where the tear duct is) of the eye .
- Sinusitis with a clear nasal discharge that can be observed when pressure is applied to the nares
- Tracheal rales (rattling sounds) and altered vocalization
- Air-sacculitis in advanced disease
In a study of B. avium in cockatiels, it was reported that the bacteria does not appear to cause disease in adult cockatiels; however, it has a severe effect on the very young cockatiel 60Symptoms of this disease that are specific only to the young and unweaned cockatiel are:
- “Sneezing with significant mucoid exudates (serious nasal discharge)
- Lethargic behavior and pasty, pale appearance
- Inflammation of the skeletal muscle responsible for opening the beak; this creates the ‘lock-jaw’ condition as the beak gradually closes over a period of 12-24 hours to a point of being ‘locked’ shut (temporomandibular rigidity)
- Constant begging for food, dehydration, and weight loss
- Protruding eyes that appear glassy and half-shut. This is due to swelling of the suborbital chamber of the infraorbital sinus, which forces the lower eyelid upward.
- Swollen appearance of the head due to inflammation of the skeletal (voluntary) muscles adjacent to the inflamed nasal cavity and infraorbital sinus.” 60
Birds may exhibit symptoms from three days to four weeks old. Breeders with these signs are considered carriers. Testing is the only way to know if a bird is a carrier. Cockatiels suffer a higher mortality rate from bordetellosis than any other species so far studied and reported. 60
At necropsy, birds have watery eyes and extensive mucus in the sinuses and trachea. There may be some hemorrhaging in the lining of the trachea. Signs of the disease usually occur seven to ten days after infection. 27
Serology tests such as ELISA and PCR will provide an antemortem diagnosis. 39 Antimicrobial agents by aerosol, injection, or in the water have not generally been effective, even though B. avium appears to be highly sensitive. “The respiratory area is difficult to medicate, and some strains of B. avium are resistant to antibiotics.” 19 A necropsy will identify lesions in upper respiratory tract, and this will confirm the diagnosis. 60

Image 68. Bordetella avium in the trachea, 7 days after infection (image courtesy M. Jackwood). 27
“Pseudomonas infection is one of the most stubborn and elusive causes of respiratory problems in birds.” 32 It is a mucoid infection, and its causes are malnutrition and poor water hygiene. It is a gram-negative, rod-like organism that is not normally found in healthy birds, but when it is, it is highly resistant to many antibiotics. The body’s warm, moist respiratory system is the perfect place for the spores to grow. This bacterium is frequently found in bathrooms, around the sink, and on the tile grout. 32
5.13.1 Testing
P. aeruginosa can usually be found in both choanal and cloacal cultures. If the numbers are low, and the bird is not showing clinical signs, treatment is usually not necessary; however, if it is found outside the GI tract, or in the choana/oropharynx, it can cause serious disease. 32
Other forms of P. aeruginosa infection are conjunctivitis and consequent keratitis and panophthalmites (inflammation involving all the tissues of the eyeball). 17

Image 69. P. aeruginosa in a chicken (image courtesy I. Dinev). 17
Pseudomonas is found in water supplies and can cause illness if it is present in high concentrations. Swamp-coolers and hoses that are allowed to sit for prolonged periods without flushing before water is dispensed can aerosolize the bacteria and be sources of contamination.49 Other sources are dirty water, dirty bowls, sipper tubes, water systems, misters, spray bottles, baths, sprouted seed, and filters that purify aviary water Cultures must be performed on taps, surfaces, and other areas that the water may contact. Even if bottled water is used, the inside of the cap may contain the bacteria. 32
The rate of recurrence of the infection is very high, making constant retesting necessary. The bacterium becomes stronger and “more resistant to antibiotics with each subsequent generation.” 32
- “Sneezing and clear or yellowish discharge from one or both nostrils
- Scratching at the nares and ears
- Conjunctivitis
- In psittacine chicks, it is often associated with chronic sinusitis and usually related to an initial aspiration event.
- Swollen sinuses around the eyes and complete obstruction of the nostrils in severe cases
- Crusty feathers around the nostrils—an early sign
- Foul-smelling diarrhea
- Necro-purulent pneumonia (pneumonia producing inflammation and pus)” 32

Image 70. Scanning electron micrograph of Pseudomonas aeruginosa bacteria (image courtesy T. Margolin) 32
The preferred treatment is with injectable antibiotics. Most adult birds have competent immune systems and can fight off the infection; however, juvenile psittacines are at greater risk of developing the infection when exposed. They are unable to contain the bacteria to the respiratory tract; therefore, “their systems may be overwhelmed and become septicemic. Hand-fed chicks will succumb to the disease if their formula water is contaminated. Water must be boiled before use and utensils must be disinfected.” 22
5.14 Bacterial Sinusitis
Bacterial sinusitis causes a collapse of the sinuses. This condition occurs most often with Pseudomonas or Bordetella sp. infections. It responds well to antibiotic therapy based on culture-and-sensitivity testing. Symptoms include “copious amounts of mucous exudate in the sinuses and requires vigorous flushing with large quantities of saline through the sinuses to dislodge the exudate.” 23 Treatment for these birds includes flushing with 60 ml of saline through each naris daily; this continues until the sinuses returned to normal. The exudate will be flushed out of the choana. The condition is most often seen in recently imported macaws. This condition may also occur if the nares become plugged with a rhinolith and the bird is prevented from breathing normally. 23

Image 71. Distended infraorbital sinus infection in a parakeet (image courtesy Louise Bauck). 26

Image 72. Sinusitis/conjunctivitis in a cockatiel with Chlamydia sinus infection (image courtesy Melbourne Bird Vet; used with permission).
Bacterial diseases are common in pet birds and should be considered in the differential list of any sick bird. Inappropriate husbandry and nutrition are often contributing factors; neonates and young birds are especially susceptible. GI and respiratory infections are most common and can lead to systemic disease. Normal bacterial flora of companion birds includes Lactobacillus, Corynebacterium, non-hemolytic Streptococcus, Micrococcus spp, and Staphylococcus epidermidis. 23
“The most commonly reported pathogens are gram-negative bacteria: Klebsiella, Pseudomonas, Aeromonas, Enterobacter, Proteus, and Citrobacter spp, E. coli, and Serratia marcescens). Pasteurella spp have been reported as possible septicemic agents in birds attacked by pet cats or rats. Mycobacterium and Chlamydia are common intracellular bacterial pathogens. Infections with Salmonella spp are occasionally seen. 23

Image 73. Serratia Marsecens on MacConkey agar (image courtesy Kayleigh Griffin; used with permission).
FREE Training to Stop Your Bird's Biting
Get FREE access to Beak School – the only system designed to train your bird. Stop behavioral problems like biting, screaming, feather plucking.
Get the Free Training“The most common gram-positive bacterial pathogens are S. aureus, S intermedius, Clostridium, Enterococcus, Streptococcus, and other Staphylococcus spp. Methicillin-resistant S. aureus (MRSA) is rare but has been documented. Mycoplasma spp have been implicated in chronic sinusitis, often found in cockatiels. This organism is difficult to culture, and the true incidence is unknown. Staphylococcus and streptococcus (especially hemolytic strains) and Bacillus spp are thought to be responsible for several dermatologic conditions in psittacine birds. Staphylococci are often isolated from lesions of pododermatitis (bumblefoot) in many avian species.26

Image 74. Streptococcus in a Gram’s stain; the red arrow is pointing to the orange-colored white blood cells, and the black arrow is pointing to streptococcus chains (image courtesy Kayleigh Griffin; used with permission).
“Clostridial organisms are common secondary invaders of damaged cloacal tissue in birds with cloacal prolapse or papillomatosis. Several specific syndromes of birds can arise from various species of clostridia. A Gram’s stain or anaerobic culture is necessary to identify these organisms. 26
“Diagnosis is based on clinical signs and results of cytologic examination and culture of tissue or swab samples. A Gram’s stain is used to identify normal flora, yeast, and spore-forming bacteria. Culture is needed to identify specific organisms and their sensitivity to antibiotics. Samples can be obtained from the respiratory, GI, urinary, and reproductive tracts. Sample sites for culture and cytology include the choanal slit, sinuses, cloaca, wounds, conjunctiva, internal organs (via ultrasound-guided, fine-needle aspirates, endoscopic examination, or surgery), and blood.” 26
5.15 Bacterial Respiratory Disease
Bacterial respiratory disease is often a stress-related phenomenon resulting from a cold environment. It may also develop secondarily to an underlying Vitamin A deficiency.
The most common pathogens involved in psittacine bacterial respiratory diseases are:
- Klebsiella
- E. coli
- Enterobacter
- Pseudomonas
- Pasteurella
- Mycoplasma
- Salmonella
- Proteus
- Serratia
- Hemophilus
- Actinobacillus 30

Image 75. Damage to the skin from mycoplasmosis (image courtesy Sofia Sangushko; used with permission)
5.15.1 Symptoms, Diagnosis, and Treatment
Clinical signs of bacterial respiratory disease may include sneezing, nasal discharge, dyspnea, lethargy, anorexia, exercise intolerance, wasting, and rarely, coughing. The clinical signs will vary according to the location of the infection, from the sinuses (upper respiratory), to the air sacs or the lungs. Tests used to diagnose bacterial respiratory disease are choanal
culture-and-sensitivity tests and radiographs. “Radiographs are extremely important in locating and characterizing the infection. 30
Important differential diagnoses include:
- Viral respiratory diseases (Amazon tracheitis virus)
- Chlamydia
- Toxic inhalants (Teflon, smoke)
- Allergies
- Fungal disease
- Dyspnea caused by abdominal distention (non-respiratory cause).” 30
Treatment involves the use of appropriate antibiotics (delivered by local application), systemic administration, and nebulization. Additional therapies include fluid therapy, Vitamin A therapy, and oxygen therapy if necessary. 30
5.16 Spontaneous Bacterial Enteritis in Psittacines
Bacterial enteritis, including necrotic bacterial enteritis, is usually associated with stress, such as transportation, relocation, introduction of a new bird or person to the home, molting, breeding/egg-laying, and weaning. Sometimes the cause is unknown. 13, 20
5.16.1 Symptoms
Clinical signs include diarrhea, dehydration, anorexia, weight loss, septicemia, and sudden death. The diagnosis is based on history, clinical signs, fecal gram stain, and cloacal culture-and-sensitivity. The fecal Gram’s stain will determine the number and type of gram-negative organisms in the feces. Other possible causes are poor diet, chlamydiosis, and hepatitis. Treatment for bacterial enteritis requires the use of appropriate antibiotics based on culture-and-sensitivity testing and fluid therapy. 20

Image 76. Digitally-colorized scanning electron micrograph of Klebsiella bacteria (image courtesy Go Pets America), http://www.gopetsamerica.com/bio/bacteria/index.aspx
The most common pathogens involved in psittacine bacterial enteritis are:
- E. coli
- Klebsiella
- Salmonella
- Pasteurella
- Pseudomonas
- Aeromonas
- Citrobacter (caused by poor water hygiene)
Other, less common organisms include:
- Enterobacter
- Proteus
- Serratia
- Yersinia
- Mycobacterium
- Chlamydophila 2O
Part VI Diagnostic Testing of Bacterial Samples
The two methods most used for identification of pathogens are Gram’s stains and cultures. Other methods are also used, but usually they are required after the sample has been tested by one or both of these methods and more information is needed about the pathogen. Today’s practitioners have at their disposal a wide variety of testing methods, from simple visual microscopic examination of impressions and unstained samples to state-of-the-art molecular diagnostic testing. These modern methods enable the clinician to identify and treat a wide range of pathogenic bacteria.
6.1 Observing the Bird for Illness
It is important that the owner pays close attention to the bird’s physical appearance so he may be able to detect early signs of bacterial or other pathogenic infections. There may be a change in the consistence of the bird’s droppings, loss of appetite, increased need for attention, increased sleeping, or other more subtle signs. If the owner waits until the bird is sitting on the bottom of the cage, he may find the is extremely ill and the situation is dire. If the owner observes any unusual signs, he needs to get the bird to the avian veterinarian immediately. He may do any number of tests, including Gram’s stains (oral and fecal smears studied under the microscope), blood samples to be sent to a lab for culture, and any other tests he deems necessary. 7
Ideally, the practitioner would wait for the results of the culture or other tests to come back from the lab, but when a bird is extremely ill, he must be treated with some medications right away, and test results often take a week or more. When the tests do come back, he may begin other treatments. The veterinarian may wish to do “antibiotic-sensitivity testing to determine the best antibiotic for that particular strain of bacteria present in the bird.” 7 The test results may mean a change to a more effective antibiotic.7
6.2 Brief Overview of Testing, Diagnosis, and Treatment
Diagnosis of bacterial disease is based on clinical signs and the results of cytology tests such as Gram’s stains and culture-and-sensitivity tests. Samples may be taken from the respiratory, GI, urinary, reproductive tracts, the choanal slit, sinus, cloaca, wounds, blood, conjunctiva, and internal organs (via ultrasound-guided, fine-needle aspirates, endoscopic examination, or surgery). 34 A Gram stain is used to identify normal flora, yeast, and spore-forming bacteria. Culture is needed to identify specific organisms and their sensitivity to antibiotics. 26 34
Antibiotics are chosen based on the results of Gram’s stains and culture tests. They should be delivered by mouth with an oral syringe since putting them in the drinking water is not a reliable method of delivery.34 Antibiotics and other medications may also be delivered via nebulization directly into a bird’s respiratory tract; this is particularly useful in cases of respiratory diseases. 50
Most bacterial infections are contagious from bird-to-bird by the droppings and water, but only a few are zoonotic to humans. 34
6.3 The Gram’s Stain Diagnostic Test
The Gram’s stain is an easy-to-use diagnostic test that has long been used in avian medicine to look for pathogens. It is quick, easy, convenient, and affordable to most clients. When combined with the physical examination and a good knowledge of avian medicine, this test is helpful in identifying early stages of many diseases. With it, the clinician is able to identify a particular pathogen or disease process before clinical signs occur. It may be used along with other clinical data gleaned from the bird’s history, the physical examination, cytological stains, cultures, and PCR tests. 15
The Gram’s stain method is named after its inventor, the Danish scientist, Hans Christian Gram (1853–1938), who developed the technique in Berlin in 1884. Gram devised his technique, not for the purpose of distinguishing one type of bacterium from another, but to make bacteria more visible in stained sections of lung tissue in humans. 41

Image 77. Hans Christian Gram, developer of the Gram’s stain (image courtesy Wikipedia: Hans Christian Gram) https://en.wikipedia.org/wiki/Gram_staining
6.3.2 The Gram’s Stain’s Function$
Gram’s staining is used to determine the presence of pathogenic bacteria in terms of their reaction to the Gram’s stain. They will be either Gram-positive and Gram-negative. The differences in staining occur due to variations in the cell-wall structures that bind the stains differently. This test is used to distinguished whether the bacteria present under the microscope are pathogens or normal, resident, beneficial bacteria. This varies among species, and interpretation requires considerable experience.10
6.3.3 Body Locations of Samples Taken for Gram’s stains
Normally, the stain is performed on samples from the gastrointestinal tract—from the choana, oral cavity, cloaca, and feces. This test is recommended for both healthy and sick birds at their annual exams. Any abnormalities warrant further diagnostic testing, including cultures and PCR tests. Other samples that may be tested with the Gram’s stain are of upper respiratory tissue, including the nares, oral cavity, sinus cavity, choanal lesions and naso-ocular discharge. Lower respiratory samples may be collected from air-sac fluids and swabs collected by endoscopic exam.15

Image 78. Gram’s staining is a method of differentiating bacterial species into two large groups: Gram-negative (red stain) and Gram-positive (blue/purple stain) (image courtesy 123rf)
Most abnormal bacteria enter through the oral cavity. Bloody mucosa or excessive mucus are reasons to perform the cytological test. The oral cavity, including the commissure (corners of the mouth) and undersides of the tongue, should be swabbed for samples and may reveal important information when tested. The gastrointestinal tract may be sampled in several different places. The oral cavity and crop may be swabbed, along with resulting fluid derived from it, and the cloaca may be swabbed to obtain fecal material. Fresh fecal samples from droppings may also be utilized. Crop, oral cavity, and cloacal swabs need to be collected carefully so that the highly vascular and friable (flaky and dry) tissues are not irritated, which can lead to bleeding. 15
Fecal samples may be viewed directly before they are stained. Motile bacteria, bacterial density, parasitic ova and cysts, urates, and undigested material are all able to be identified. With granulomas (a mass or nodule of inflamed or infected tissue) and skin lesions, the tissue under the wounds can be sampled and stained. Other areas that can be tested and analyzed are the feather pulp (inside of a blood feather) and feather follicles. 15

Image 79. This picture is showing a negative gram stain test and a positive Gram’s stain test. A Gram’s stain test is performed by putting alcohol on the bacteria. It will either turn a violet color or a pink red color. If it’s violet, the test is positive; if it’s a red-pink color, the test is negative. A positive result means the bacteria will have a thick cell wall, a negative result that means the bacteria has a thinner cell wall. Pseudomonas fluorescens will be negative if a Gram’s stain test is performed (image courtesy SA Site for Science).
6.3.4 Further Testing Determined by the Results of the Gram’s Stain
One benefit of the Gram’s stain is to prompt the clinician to pursue other diagnostic assays if he is not satisfied with the results of the Gram’s stain.15 For example, if inflammatory cells, abnormal red blood cells, or other abnormal cells are suspected from the Gram’s stain, the practitioner will want to perform another cytological stain or possibly a culture-and-sensitivity test. Further tests may include a Polymerase Chain Reaction (PCR), a molecular diagnostic test. 15

Image 80. Gram’s Staining. A Gram’s stain of mixed Staphylococcus aureus (S. aureus, Gram-positive cocci, in purple) and Escherichia coli (E. coli, Gram-negative bacilli, in red), the most common Gram-stain-reference bacteria (image courtesy Wikipedia). https://en.wikipedia.org/wiki/Gram_staining)
6.3.5 What information does the practitioner glean from the Gram’s stain that cultures cannot provide?
“Cultures alone cannot identify many important aspects in a sample that the Gram’s stain may reveal. The culture cannot identify:
- Numbers of yeast, fungal hyphae, and budding yeast
- Sporulated rods, spirochetes, megabacteria (Macrorhabdus ornithogaster, a fungus), protozoa, and the relative number and percentages of bacteria
- Pathogenic bacteria which have special growth requirements, e.g., Pasturella species.” 15
If the bacterial population fails to take up the blue-purple part of the Gram’s stain, it will only retain the red counterstain and therefore appear red or Gram-negative. Gram-negative organisms are more likely to be pathogenic in birds, but not always.10Brown

Image 81. This Gram-negative smear (1000x magnificaion) was taken from a cultured sample of a sinus swab in a cockatiel with sinusitis (sinus infection) and shows both characteristic red Gram-negative bacilli (rod shaped) and cocci (round) bacterial organisms (image courtesy D. Brown). 10
Bacteria can be identified as being pathogenic based on their staining characteristics by using a Gram’s stain. Since these bacteria have taken up the blue-purple part of the stain, they are Gram-positive. Most Gram-positive organisms are beneficial and normal in most parrots, but some cause disease. 10

Image 82. This is a Gram-positive smear at 1000x magnification. It was taken from a cultured sample of a routine sinus swab in a cockatiel and shows both characteristic blue-purple, Gram-positive bacilli (rod-shaped) and cocci (round) bacterial organisms (image courtesy D. Brown).10
6.3.8 Images of Various Bacteria after Gram’s staining
6.3.8.1 Appearance of Mycobacterium organism. Some Gram-positive bacteria can be pathogenic, such as the Mycobacterium organism, a rod-shaped bacterium.

Image 83. This image shows liver tissue with avian tuberculosis bacterial organisms, specifically Mycobacterium spp (a Gram-positive, aerobic bacteria, occurring as slightly curved or straight rods.) The sample has been stained red-purple and viewed at 400x magnification. It is from a long-tailed finch (image courtesy D. Brown)10 Brown
6.3.8.2 Appearance of the Spiral and Spirillum Bacterium

Image 84. Spirillum bacteria, a variation of the spiral bacteria as it appears in a Gram’s stain. They have a corkscrew appearance (image courtesy Imarcade).
Imarcade.com http://imgarcade.com/spirillum-bacteria-under-microscope.html)
6.3.8.3 Appearance of the Coccus Bacterium

Image 85. Cocci, or round-shaped bacteria in a Gram’s stain (image courtesy Imarcade). http://imgarcade.com/coccus-bacteria-under-microscope.html
6.3.8.4 Appearance of Cocci in a Gram’s Stain.
In Some Cocci Infections, the Bacteria Form Chains

Image 86. Streptococcus pneumoniae, a Gram-positive bacterium (image courtesy Imarcade). http://imgarcade.com/cocci-bacteria-under-microscope.html
6.3.8.5 Appearance of Rod-shaped Bacteria

Image 87. Rod-shaped Bacteria. Colored scanning electron micrograph (SEM) of rod-shaped (bacillus) bacteria. The tubes connecting the bacteria are pili, which are used to transfer genetic material between bacteria in a process known as conjunction (Image courtesy Science Photo Library)
6.3.9 The Gram’s Stain Method of Bacteria Identification
The Gram’s stain is a test used to identify bacteria by the composition of their cell walls. Oral and fecal samples are put through a staining process after which the practitioner looks for the distribution of various bacteria. Bacteria are first stained with a purple dye called “crystal violet” which specifically binds to peptidoglycan, a complex structure of amino acids and sugars found in the cell wall. This is followed by a series of steps that ultimately removes any unbound or loosely bound crystal violet. 51, 54.
Then the cells are stained with a second red-colored dye called safranin. Gram-positive bacteria stain purple because their cell walls are rich in peptidoglycan. Gram-negative bacteria, whose cells walls have two layers, take on a red coloring. The outer layer of lipids does not bind strongly to crystal violet, and the dye is easily washed away during the staining process. For example, Streptococcus pneumoniae, which causes pneumonia, is a Gram-positive bacterium, while E.coli and Vibrio cholerae (which causes cholera), are Gram-negative bacteria. 11
Sometimes, while the clinician is performing the Gram’s-staining technique, there will be errors in the process, making interpretation difficult. The slide may be overheated, or the sample may be decolorized; these are the most commonly found errors. The technique must be uniform, and fresh samples must be used.15
Certain factors influence the interpretation and effectiveness of the Gram’s stain:
- Age and species of the bird
- Diet
- Cage hygiene
- Husbandry practices. 15
6.3.10 Discerning Normal from Abnormal Bacteria in a Gram’s stain.
Clinicians need to be able to judge normal from abnormal bacteria and know the number and ratios of normal bacteria for a particular species. Normal oral and GI flora from psittacine birds consist primarily of Gram-positive rods and cocci. An occasional Gram-negative rod or fungal organism (yeast) is normal, but if there is an abundance of these, or they are frequently seen in successive stains, they are considered abnormal. 15
Normally, the choanal slit (narrow opening in the top of the mouth) of birds contains squamous epithelial cells and a slight-to-moderate number of bacteria. They usually stain Gram-positive. Abnormal stains may contain inflammatory cells, yeasts, fungal hyphae (long, branching filamentous structures of a fungus), or a large number of Gram-negative rods or cocci. 15
“Epithelial cells form the epithelium, which is a membranous tissue that covers the internal area of organs and other internal surfaces of the body and also covers the external skin. If the stained sample contains few epithelial cells and fewer-than-normal numbers of bacteria, that is a cause for concern. Ideally, there should be no more than 10% of Gram-negative bacteria in psittacines. An increase of more than 10% of Gram-negative bacteria is not normal. The more Gram-negative bacteria found, the more pathogenic the situation. Just because there are no Gram-negative bacteria in a sample does not mean they are not present elsewhere in the area of the body from which the sample was taken. Any abnormal findings are cause for additional testing, such as culture-and-sensitivity tests and a complete blood count (CBC), especially the white-blood-cell count (WBC).” 15
Once he gets the results of the Gram’s stain back, the practitioner will record the results of the test.
Blood tests can be used to check for serum antibody levels to certain organisms, including bacteria. PCR can also be used but is generally run on tissue swabs, not blood. Bacteria in the blood indicates sepsis. About 50% of septic cases die.
The feather pulp and skin swabs are performed to check to see what kinds of organisms are present in that area. They may or may not represent the cause of a skin or feather pulp problem. R. Dahlhausen
6.3.11 Diagnosing from the Gram’s Stain
Gram’s stains provide valuable information to the clinician; however, they do not constitute a diagnosis; neither can they assist in the diagnosis of other difficulties the bird may have, such as a respiratory problem or injury. 18
Diagnosis depends on other screenings in addition to the Gram’s stain. The Gram’s stain is a valuable diagnostic screening test in both well and sick birds, but other factors need to be taken into consideration, such as the bird’s history and the results of the culture and CBC tests.15
The bird owner needs to pay close attention to the bird’s physical appearance. If the bird shows signs of illness, the owner needs to make an appointment with the veterinarian and have these tests performed. It takes a while for the results to come in many instances; meanwhile, as the clinician and owner wait, the bird continues to become more and more ill. Before he even knows the information gleaned from the tests, he must prescribe medication to treat the symptoms at that time, based on his differential diagnoses (possible reasons for illness). He may prescribe a broad-spectrum antibiotic that will aid in recovery until he is able to do sensitivity testing and prescribe the correct antibiotic for the illness.
6.3.12 Interpretation of Gram’s Stain Results
Interpretation of what is visible on the Gram’s stains is not easy; it takes experience to sort through all that is there and find the pathogen responsible for the bird’s illness. Many other areas must be explored as well; the bird’s history and symptoms are of great importance. The following images and their explanations are examples of documentation of the results of the Gram’s stains.
KEY: Hx = History, CS = Clinical Signs, GS = Gram’s stain results Rx = Therapy
I
Image 88. Four-year-old male Budgerigar, Apparently healthy bird, fed a pelleted diet. CS = none. Gram Stain results = Normal distribution of organisms: 157 total bacteria per field, 70% gram-positive rods, 30% gram-positive cocci, 0 gram-negative bacteria, 0 yeast. Digestion of food is complete (image courtesy Clinical Avian Medicine, Harrison-Lightfoot).
Image 89. African grey parrot, 4 years old, sex unknown: Hx = Intermittent vomiting or loose stool, not as playful. GS = 400 bacteria per oil field, 95% Gram-positive short rods, 5% Gram-positive rods, 0 yeast. Overgrowth of intestinal bacteria, enterotoxaemia (a condition induced by the absorption of large volumes of toxins produced by Clostridium perfringens from the intestines), malnutrition. Rx = Aggressive (image courtesy Clinical Avian Medicine, Harrison-Lightfoot).
Image 90. Severe macaw, 7 years old, sex unknown: Hx = Depressed, not eating, weak. CS = underweight, scant feces, dark yellow urine and urates, malcolored feathers. GS = 200 bacteria per field, 1% gram-positive rods, 0% gram-positive cocci, 98% gram-negative rods. Rx = Aggressive (image courtesy Clinical Avian Medicine, Harrison-Lightfoot).
Image 91. Umbrella cockatoo, 6-year-old female: Hx = Exposure to carnivorous pets, seed only diet. CS = Fetid stool, weight loss, passing undigested food. GS = 200 bacteria per field, 10% gram-positive rods, 90% gram-negative rods, of which 50% are Clostridium sp. Rx = Aggressive (image courtesy Clinical Avian Medicine, Harrison-Lightfoot).
Cultures are done along with the analysis of growth on certain media plates and certain biochemical tests and morphology to identify the bacteria involved. The organism can be grown on a special media plate with multiple discs, each containing a certain antibiotic. This is the sensitivity part of the test. The Zone of Inhibition of growth around the disc determines if the organism is sensitive or not to that antibiotic.
Bob Dahlhausen
Sensitivity testing
Image 92. Moluccan cockatoo, 7-year-old male: CS = smelly stool. GS = 50 bacteria per field, 90% gram-positive rods, 10% gram-positive cocci, 30 Clostridium sp. organisms. Rx = Aggressive (image courtesy Clinical Avian Medicine, Harrison-Lightfoot).

Image 93. “Zone of Inhibition” assay on a culture plate to define which antibiotic works the best. The size of the zone is relative to the potency of the antibiotic. The “Zone of Inhibition” means that the bactericidal or bacteriostatic agent has either inhibited or killed the organisms that were spread on the plate, and that those organisms are susceptible to that agent
(image courtesy Toxikon Services). http://www.toxikon.be/services/Microbiology_Pharma_Biotech.cfm)
6.4 Other Stains Used in the Diagnostic Process
These are the routine stains used in avian cytology, histopathology, and histology. Each of these stains is used for a particular purpose, depending on what the bird is being tested for.
- Wright’s stain
- Wright-Giemsa stain
- Giemsa Stains
- Quick or Stat Stains
- New Methylene blue stain
- Special stains
- Acid-fast stain
- Gram’s stain
- Macchiavello’s stain
- Modified Gimenez stain
- Natt and Herrick’s solution
- Sudan III and Sudan IV stains
“Most of these stains have been in use for many years. The cytology and histopathology stains for birds are going to be the same as for animals and people. The same is true for hematology. Wright-Giemsa stain or a Quick or Stat stain like Dif-Qwik are most commonly used in the clinic setting. Most of the others are special stains and are used by laboratories for special purposes. New Methylene Blue stain is used in cytology and histopathology, typically for staining immature red blood cells. 15
“Hematologic stains. There are a number of special stains employed to identify specific inflammatory cells seen in peripheral blood and tissues. These include the all-purpose Wright-Giemas and Giemsa stains, leukocyte alkaline phosphatase (LAP), tartrate-resistant acid phosphatase (TRAP), and myeloperoxidase (MPO). 15
“There are a variety of “Romanowsky-type” stains with mixtures of methylene blue, azure, and eosin compounds. Among these are the giemsa stain and the Wright’s stain (or Wright-Giemsa stain). The latter is utilized to stain peripheral blood smears. The giemsa stain can be helpful for identifying components in a variety of tissues.15
“One property of methylene blue and toluidine blue dyes is metachromasia. This means that a tissue component stains a different color than the dye itself. For example, mast cell granules, cartilage, mucin, and amyloid will stain purple and not blue, which is helpful in identifying these components. 15
“Fat Stains: Lipids cannot be demonstrated in routine tissue sections, as during processing the tissue and clearing, lipids will be dissolved. Lipids are routinely demonstrated in frozen sections or cryostat sections. 15
“Special fat stains used are:
- Oil Red O
- Sudan III
- Sudan IV
- Sudan Black
- Osmium tetroxide
“For more information on stains, the reader may research the individual stain on Wikipedia. There are sites which contain specifics about the individual stains.
“Other sites which offer information about stains are::
- https://webpath.med.utah.edu/HISTHTML/STAINS/STAINS.html
- https://www.histopathology.guru/?s=stains”
(All information on stains from Bob Dahlhausen, personal communication.)
6.5 Culture-and-Sensitivity Diagnostic Testing
A culture refers to the propagation of living organisms or the living tissue cells in special media conducive to their growth. It is also the product of such propagation. It is used when birds are suspected of having a bacterial infection and the Gram’s stain does not yield sufficient information. 8
6.5.1 Culture-and-Sensitivity Testing Methodology
To perform the test, a sterile swab of the body fluid in question is obtained and streaked on a laboratory plate. These samples can be from sinus drainage, fecal and oral material, or pus. The plate is a shallow, flat receptacle filled with agar; this provides the nourishment that allows the suspected bacteria to grow. The culture plate is then placed in an incubator overnight. By the next day, bacterial growth is usually visible. If insufficient growth has occurred, the organism may be placed onto a different growth medium and incubated for another twenty-four-hour period. This way, the culture process allows the specific bacteria infecting the bird to be identified. 25
Once the pathogenic organism has been identified, the clinician will perform sensitivity testing to determine the sample’s response to different antibiotics. “Sensitivity” refers to the ability of the one or more of the antibiotics to kill the bacterium. If the bacterium is killed by the antibiotic, it is “sensitive” to it.25
“To test for sensitivity, antibiotic-impregnated paper discs are placed on the surface of the culture plate on which the bacteria are growing. After a period of time, the plates are observed for bacterial ‘kill off.’ This is manifested by a clear zone (Zone of Inhibition) around one or more the antibiotic discs, indicating that the bacteria are unable to live and grow in the presence of that particular antibiotic.” 25
Not all bacteria are killed by all antibiotics. The veterinarian will choose the most effective antibiotic for the bird’s infection, based on the results of the culture-and-sensitivity testing. 25

Image 94. Bacterial growth on a petri dish (image courtesy https://uk.vwr.com/store/content/externalContentPage.jsp?path=/uk.vwr.com/en_GB/microbiology_segment.jsp).

Image 95. Colony of bacteria in culture medium plate (image courtesy 123rf). https://www.123rf.com/stock-photo/bacteria_culture.html

Image 96. Agar as a medium for bacterial growth
(image courtesy Just We Diminute). http://www.justwedeminute.com/2010/04/ewww-growing-bacteria-for-science.html)
6.5.2 Commonly Found Bacteria in Cultures
Normal fecal bacteria cultured from healthy birds include:
- Gram-positive bacilli (Lactobacillus spp., Bacillus spp., Corynebacterium spp., and Streptomyces) Older birds tend to have more Corynebacterium and less Lactobacillus than juvenile birds.
- Gram-positive cocci (Staphylococcus epidermidis, Streptococcus spp., Aerococcus spp., and Micrococcus spp.)
- Escherichia coli is commonly recovered from cockatoos, but less commonly in other species.
- Gram-negative bacteria occasionally found in clinically normal birds include: Enterobacter, Klebsiella, Citrobacter, Pasteurella, and Moraxella spp.
- While some Pseudomonas spp. have been recovered from healthy birds, P. aeruginosa is rarely found in healthy birds.
- Isolation of Proteus, Salmonella, Pseudomonas, Klebsiella, Listeria, Erysipelothrix, and hemolytic Staphylococcus aureus is clinically significant in sick birds.”
Cultures from other sites such as the eyes, ears, and choana usually show similar results. Any heavy overgrowth of bacteria warrants further investigation.” 18
6.6 Identifying the Pathogens Using Cytology and Histopathology
There are some differences between cytology and histopathology. “Cytology is done with a swab or fluid from a fine-needle aspirate (FNA). It does not contain solid tissue, so it cannot assess tissue architecture, just cell types present. Histopathology is tissue collected by biopsy or necropsy. For example, a crop swab or crop wash yields cytology and culture samples but cannot evaluate the health of the crop tissue. Histopathology of the crop evaluates the crop wall itself. Histopathology is not used for culture as it is placed in formaldehyde (Formalin), but one can culture the sample before placing it in Formalin. Both can see bacteria and cells. Cytology images consist of the whole organism spread out across a slide, while histopathology uses cut samples, usually tissue blocks, so they will look a little different. Histopathology is not always of disease samples, but it is some form of tissue, so any bacteria may be embedded in it (typically). The results will also depend on which stain is used.” (Bart Huber, personal communication; used with permission).
6.6.1 Cytology
Cytology is the study of the structure, function and chemistry of cells. It deals directly with the structural and functional organization of cells and also with metabolism, ontogenetic differentiation (the development of an individual organism from inception to maturity and comparing it to that of another organism), heredity, and phylogeny (the evolutionary history of an organism). 20
Cytology is the study of cellular anatomy, physiology, pathology, and chemistry, and it provides valuable information about the disease process being examined. Only a very small sampling of cells is required so it doesn’t further traumatize the already-compromised tissue. 8
FREE Training to Stop Your Bird's Biting
Get FREE access to Beak School – the only system designed to train your bird. Stop behavioral problems like biting, screaming, feather plucking.
Get the Free TrainingCytological tests can be used to identify cancer cells, the sex of birds, and to give information on the nature of infectious processes, particularly whether they are acute or chronic. Cells from any part of the body may be examined, e.g., the digestive and respiratory tracts, oral and fecal areas, skin, and joints. 8

Image 97. Cytology of normal bacterial microflora in a cloacal sample from a Yellow-fronted Amazon parrot using Gram’s stain (image courtesy Terry Campbell: Avian Hematology and Cytology. Iowa State Univ. Press, 1988, p. 50).

Image 98. Chronic active sinusitis in a Scarlet-chested Parrot. Small, round purple intracytoplasmic inclusions (center) are seen in many of the cells. A presumptive diagnosis of chlamydiosis was made based on these findings and the clinical signs. Chlamydiae were isolated from the sample. The sample was stained with Diff Quick (image courtesy Terry Campbell: Avian Hematology and Cytology. Iowa State Univ. Press, 1988, p. 50).
6.6.2 Histopathology
Histopathology is the microscopic examination of tissue changes caused by disease. It refers to the examination of a biopsy or surgical specimen by a pathologist after the specimen has been processed and histological sections have been placed onto glass slides.. 3, 21
Many diseases cannot be identified by simple light microscopy of organ contents. They may require histopathology. This is a process by which very fine sections of suspect tissue are sliced, stained, and prepared for examination. They may be stained and examined immediately; other times, they may need to be cultured before they can be stained and examined. Gram’s stains are usually performed first, then, if necessary, other methods of testing may be utilized. 9
6.6.3 Methods of Obtaining Cell Samples for Cytology and Histopathology:
- Swab: In an exposed area of the body, such as an open wound, a swab or scraping of the area will be taken and its contents spread on a slide. 8
- Impression smears, also called “contact smears” from skin and internal organs. The slide will be pressed directly onto the affected area to obtain the needed cells. 8
- Fine-needle aspirate of masses or organs: If a sample is needed from an internal area of the body (e.g., fluid in the abdomen), a sterile needle and syringe will be utilized to remove the necessary sample. 9
- Saline wash: “If samples are needed from the crop, air-sac, or trachea, sterile saline will be instilled into these areas and then removed by sterile syringe and tubing. The saline solution will then contain numbers of cells that can be examined.” 4, 7
- Sinus aspirates, often performed with saline washes. 7
- Abdominocentesis: introduction of a needle into the abdominal cavity in order to reach fluid. 7
- Arthrocentesis: using a syringe to collect synovial fluid from a joint capsule. It is also known as joint aspiration 7
- Scrapings from the palpebral conjunctiva or cornea of the eyes, from the oral cavity, or tissues that normally yield poor cellular samples. 7
6.7 Other Testing Methods
Many types of tests will indicate the presence of bacteria. Lab tests for avian species are divided into several basic groups:
- Indicators of immune system activity: the CBC and EPH (electrophoresis: A method of separating substances, especially proteins, and analyzing molecular structure based on the rate of movement of each component while under the influence of an electric field.) 42
- Serum biochemistries (blood tests): indicate the condition or function of various organ systems.
- Serology (Gram’s stains and cultures): tests for antibodies to various diseases. Antibodies are small proteins that circulate in the bloodstream. They are part of the body’s immune system and are made by B lymphocyte while blood cells. Antibodies attach to proteins and other foreign chemicals in the body which they recognize as abnormal. The foreign proteins and chemicals that antibodies attach to are called “antigens.” 42
- Antigen-detection tests: tests for the antigens specific to infectious agents. Some tests can identify the antigen on the surface of some bacteria. 25
- Miscellaneous: randomly utilized tests such as urinalysis. 25
Conclusion
The devastating effects of bacterial diseases on avian populations are enormous. As science continues to explore and understand the number and function of current bacterial pathogens, newly discovered bacteria await analysis and description. Bacteria that are harmful to birds, both pet and wild, are unable to be identified without cytology and histopathology to define them.
Care must be taken by owners to keep the aviaries scrupulously clean, watch for signs of infection, and obtain proper diagnoses and treatments from avian veterinarians as soon as possible. Therapeutics provide the optimum chance of eliminating the disease if it is caught early. Bacteria travel and reproduce quickly, so there is no time to waste. Constant observation of the bird and his environment is of utmost importance.
References
1. Anderson L. Antibiotics Guide. Drugs.com. https://www.drugs.com/article/antibiotics.html x
2. Avian Biotech. Clostridium. Avianbiotech.com. 1995
http://www.avianbiotech.com/diseases/clostridium.htm
3. Avian Biotech. Mycobacterium avium, or Avian Tuberculosis.
Avianbiotech.com http://www.avianbiotech.com/Diseases/AvianTuberculosis.htm
4. Avian Biotech. Salmonella. http://www.avianbiotech.com/diseases/salmonella.htm
5. Bacteria. The Encyclopedia of Life. http://www.eol.org/info/455
6. Bacterial Diseases of Pet Birds. Merck Veterinary Manual.
http://www.merckvetmanual.com/exotic-and-laboratory-animals/pet-birds/bacterial-diseases-of-pet-birds#v4631675
7 Birds and Antibiotics. Parrot Parrot
Birds and Antibiotics
8. Blood D. et al. Saunders Comprehensive Veterinary Dictionary, Third Ed. Saunders/Elsevier 2007
9. Briscoe JA, et al. Methicillin-Resistant Staphylococcus aureus–Associated Dermatitis in a Congo African Grey Parrot (Psittacus erithacus erithacus) (Abstract). Journal Avian Med and Surgery December, 2008: Vol. 22, Issue 4 (Dec 2008), pp. 336-343
10. Brown D. Histopathology. Under the Microscope. ABK Pub. 2003
11. Brue R. Nutrition. In: Avian Medicine: Principles and Application, Ritchie, Harrison, p. 65
12. Campylobacter. Go Pets America. http://www.gopetsamerica.com/bio/bacteria/campylobacter.aspx
13. Cannon MJ, A Guide to Basic Health & Disease in Birds. ABK Publications. 2002
14. Clubb S. and Flammer K. Preventing Bacterial Disease in the Home. In: Avian Medicine: Principles and Application. Ed. Harrison. Spix Pub. Co. 2006, pp. 54-58
15. Dahlhausen Bob, et. al. Diagnosis of Mycobacterial Infections in the Exotic Pet Patient with Emphasis on Birds. Vet Clin Exot Anim These are the routine stains used in avian cytology, histopathology, and histology. Each of these stains is used for a particular purpose, depending on what the bird is being tested for. Vol.15 (2012) 71–83, vetexotic.theclinics.com © 2012 Pub Elsevier, Inc.
16. Difference Between Bactericidal and Bacteriostatic. Differencebetween.com. 2013
Difference Between Bactericidal and Bacteriostatic
17. Dinev I. Diseases of Poultry. http://kenanaonline.com/files/0032/32316/paratyphoid-infections.htm)
18. Doneley B. Central Nervous System Disorders. Avian Medicine and Surgery in Practice. Manson Pub. Inc. 2011 p. 205, 209, 211
19. Doolan M. Zoonotic Bacterial Infections from Human to Bird. Cockatoo Message Board. www.mytoos.com
20. Durairaj V. and Clark D. Necrotic Enteritis. Avian Advice Newsletter In: The Poultry Site, 2007 http://www.thepoultrysite.com/articles/846/necrotic-enteritis/
21. Fiskett RA, Reavill DR. Disease Conditions and Clinical Signs of Pet Birds. Proc Assn Avian Vet 2004, pp.245-266
22. Flammer K. Treatment regimens. In: Avian Medicine: Principles and Application. Ritchie, Harrison, and Harrison Ed. Harrison. Spix Pub. Co. 2006 p. 437
23. Forbes N, Altman R. Self-assessment Color Review of Avian Medicine. Manson Publ./The Veterinary Press. 1998
24. Gerloch H. Defense Mechanisms of the Avian Host. In: Avian Medicine: Principles and Applications. Ritchie, Harrison, and Harrison Ed. Harrison. Spix Pub. Co. 2006 p. 149
25. Harris D. Clinical tests. Handbook of Avian Medicine, 2nd Ed., Ed. T. Tully. Saunders/Elsevier Pub. 2009
26. Hoppes SM. Bacterial Diseases of Pet Birds, In: Merck Veterinary Manual. Pub: Merck, Share, and Dohme. 2016 p. 14, http://www.merckvetmanual.com/exotic-and-laboratory-animals/pet-birds/bacterial-diseases-of-pet-birds.
27. Jackwood M. Overview of Bordetellosis in Poultry. In: Merck Vet Manual. Pub: Merck, Share, and Dohme. 2016. http://www.merckvetmanual.com/poultry/bordetellosis/overview-of-bordetellosis-in-poultry
28. Jenkins J. Diseases of Small Passerine Birds. Avian and Exotic Animal Hospital. http://www.drexotic.com/diseases-of-small-passerine-birds/
29. Jilani. Difference Between Aerobic and Anaerobic Bacteria. DifferenceBetween.net. April 18, 2010 < http://www.differencebetween.net/science/difference-between-aerobic-and-anaerobic-bacteria/
30. Kaufman G. Bacterial Diseases. Lectures Zoo Med: Psittacine Medicine (2008)
http://ocw.tufts.edu/Content/60/lecturenotes/832349
31. Kratz R, Siegried D. Biodiversity and Classification, and Fighting Back: Human Defenses. Biology for Dummies, 2nd Ed. Pub. John Wiley & Sons, Inc. 2010 p. 148-149, 260-261
32. Margolin T. Pseudomonas. In: Hot Spot for Birds. http://www.multiscope.com/hotspot/articles/pseudomonas.htm
33. Marshall R. Psittacosis. In: Beauty of Birds website. https://www.beautyofbirds.com/psittacosis.html
34. Marshall R. What is a bacterial infection? In: Beauty of Birds. https://www.beautyofbirds.com/bacterialinfection.html
35. Medical Importance of Bacteria. Go Pets America http://www.gopetsamerica.com/bio/bacteria/index.aspx
36. Microbewiki. Bordatella. https://microbewiki.kenyon.edu/index.php/Bordetella
37. Miesle, J. The danger of cats, in the files of “The Science of Avian Health.”
38. Miesle Terrence.J., M.S. Senior Chemist, Sensient Foods, personal communication
39. Mikesh L. Five different types of bacteria. Livestrong 2017 http://www.livestrong.com/article/117677-five-different-types-bacteria/
40. Morishita T. Overview of Streptococcosis in Poultry. Merck Veterinary Manual, 2018 © 2018 Merck Sharp & Dohme Corp. http://www.merckvetmanual.com/poultry/streptococcosis/overview-of-streptococcosis-in-poultry
41. Optical Microscopy. Wikipedia https://en.wikipedia.org/wiki/Microscopy
42. Payne J. Antibody and Antigen tests. Patient. 2015 https://patient.info/health/antibody-and-antigen-tests
43. Ritchie B, Dreesen D. Avian Zoonoses: Proven and Potential Diseases, Part I: Bacterial and Parasitic Diseases. In: Practical Avian Medicine, The Compendium Collection. Ed: Heidi L. Hoefer. Pub: Veterinary Learning Systems, 1997.
44. Rodgers W. Bacterial Contamination of Food, Animal Hospitals USA. http://www.animalhospitals-usa.com/birds/bird-diseases/bacterial-culture.html
45. Staphylococcus. Go Pets America. http://www.gopetsamerica.com/bio/bacteria/staphylococcus.aspx
46. Speer B. Diagnosis and Management of Key Infectious Diseases. Proc Latin Am Vet Conf. Reprinted in the IVIS website with the permission of the LAVC, http://www.ivis.org/ 2009, p. 330-339
47. Spiral Bacteria. Wikipedia https://en.wikipedia.org/wiki/Spiral_bacteria
48. Stephens E., Antibiotics. E Medicine Health 2016
http://www.emedicinehealth.com/antibiotics/page2_em.htm
49. Styles D. Bacterial Disease And Antimicrobial Therapy In Avian Species. Proc N. Am Vet. Community. Reprinted in the IVIS website with the permission of the NAVC 2005
50. Sweat R. Treatments Recommended For Avian Respiratory Problems. Veterinary Practice News 2009 http://www.veterinarypracticenews.com/Vet-Dept/Avian-Exotic-Dept/Avian-Respiratory-Problem-Treatments/
51. The Light Microscope. Experimental Biosciences, Rice University Press. (http://www.ruf.rice.edu/~bioslabs/methods/microscopy/microscopy.html)
52. Tlaskalova-Hogenova H. Commensal bacteria (normal microflora), mucosal immunity and chronic inflammatory and autoimmune diseases. Abstract In: Immunology Letters, Volume 93, Issues 2–3, 15 May 2004, Elsevier Pub. Co. Pages 97-108 http://www.sciencedirect.com/science/article/pii/S0165247804000379
53. Todd E.C.D. History, Science and Methods. In: Encyclopedia of Food Safety, Science Direct, 2014
54. Vidyasagar A. What are Bacteria? Live Science. https://www.livescience.com/51641-bacteria.html 2015
55. Walker C. Streptococcal Infections in birds. Melbourne Bird Vet Clinic. 2015 http://www.melbournebirdvet.com/streptococcus-infections-in-birds.aspx
56. Weir S. E. Coli Infection in Pigeons. The Pigeon Insider. 2002
E. Coli Infection in Pigeons
57. What is the difference between cytology and histology? DifferenceBetween.Com. June 7, 2012. http://www.differencebetween.com/differences-between-histology-and-vs-cytology/
58. What is the difference between true and opportunistic pathogens? Answers.com (http://www.answers.com/topic/opportunistic)
59. Wikipedia. Histopathology. 2017 https://en.wikipedia.org/wiki/Histopathology
60. Wikivet. Bordetella Avium. https://en.wikivet.net/Bordetella_avium
61. Wissman M. Bacterial Issues In Pet Birds. www.exoticpetvet.net. 2009
Appendix A, from p. 31
Staph vs MRSA – What’s the Difference?
Staph vs MRSA – What’s the Difference? (staph-infection-resources.com) Image courtesy Staph Infection Resources
The differences between MRSA versus S. aureus are significant when it comes to antibiotics and infection control. The key differences listed below play a big role in treatment effectiveness and how quickly a person recovers. In many other ways, however, the differences can be minimal between these two infections.
How they are alike
- The symptoms of MRSA vs S. aureus are very similar. MRSA can be more virulent and more invasive than S. aureus. The rare and deadly form of these infections, called “flesh eating disease” (necrotizing fasciitis,) is more commonly caused by MRSA rather than S. aureus.
- In photos, MRSA and S. aureus look nearly identical. Because they look so alike, the best way to tell them apart is to get tested.
- Both of these infections are also contagious and can easily spread from person-to-person or from contaminated surfaces.
- The most effectively used alternative remedies can work equally well for both S. aureus and MRSA. The lack of resistance issues with most natural and alternative therapies is one of their big benefits.
- MRSA and S. aureus are the same species of bacteria. MRSA (short for Methicillin Resistant Staphylococcus Aureus) is just a special kind of Staph (short for Staphylococcus aureus, or more commonly Staph aureus). The main differences between the two are listed below.
Key differences
- The big difference between S. aureus and MRSA is with antibiotic treatments. MRSA is resistant to most commonly used drugs, but S. aureus is much less resistant. This is an important difference when it comes to choosing the right antibiotic for an infection. MRSA also tends to result in longer, more expensive hospital stays than S. aureus.
- S. aureus is more common than MRSA. Around a third of the people in the U.S. are carriers of S. aureus bacteria on their skin, while fewer than 5% carry MRSA. S. aureus bacteria are extant and a natural part of the environment. Thankfully, MRSA is still mostly confined to hospitals and healthcare environments, but it has been growing rapidly in the community over the last decade or so.
- MRSA can be harder to kill on surfaces than S. aureus. For some disinfectants, such as silver-based products, the kill time for MRSA can be two or three times the kill time for S. aureus.

S. aureus as MRSA (image courtesy CDC) https://www.cdc.gov/mrsa/community/photos/photo-mrsa-1.html).
Appendix B: from p. 34
Case Study: Author’s rescued cockatiel, Boots. Severe sinus and eye bacterial infection.
The attending veterinarian is Dr. Bob Dahlhausen.
May 25, 2021. The bird arrived at the author’s home. Weight: 100 g. There was a heavy scab over the right eye, pushing skin and bone out, away from the eye. I removed the scab and blood and other fluids emerged from the eye. The next day I took him to the avian veterinarian. He had had sinusitis for a long period of time, and this led to the globe collapsing and the lens beginning to calcify. Dr. Dahlhausen injected an antibiotic directly into the bulbar conjunctiva under the globe. The antibodies had infused deposits in the lens.

Severe sinus infection in the author’s cockatiel. The bacteria was Streptococcus aureus. The image was taken after the scab was removed; the orbit had collapsed, and the eye had sunk down under the skin. For several days, the tissue leaked blood and fluid. The scab had pushed the skin and feathers away from the eye in a circular manner, and a hard ring of the forced tissue remains (see black arrow) (image courtesy J. Miesle).

Severe sinus infection in a cockatiel. This is a bird with a similar condition. The scab is still on this bird’s eye, and it gives you an idea of what the author’s bird looked like when she took him in (image courtesy Melbourne Bird Vet; used with permission).
He was to be kept separated until the results of chlamydia test came back. Everything in the respiratory tract was inflamed, and there was undigested fiber in the stool. Gram’s stains showed pus and gram-positive bacteria. The eye could not be removed because the optic nerve is short, and any pressure or tension would kill the bird. He would manage it medically. Boots has no vision in the eye. I was to put warm compresses on it to sooth it and prevent a recurrence of it scabbing over. I was also to put drops of saline solution in the eye 3-4 times a day for at least 2 weeks, probably much longer, to prevent the eye from closing up. If that happened, the infection could start up again since the fluid would not be able to drain. He also gave me an antibiotic cream to put on the eye daily. Boots was started on Azithromycin and that continued for several weeks. His weight was 100 g. when he was taken in. I had begun giving him Emeraid Nutritional Supplement, both Omnivore and Carnivore, plus vitamins, several times a day from the first day on. He continues to receive this to the present day and it will continue indefinitely. His left eye has a large cataract on it, preventing sight. He is, for the most part, blind.
The chlamydia test was negative. By the 31st, his weight had plummeted to 80 grams and he was losing more each day. He had no appetite.
June 4: Boots’ weight was down to 73 g. We made an emergency visit to Dr. Dahlhausen at 8 a.m. He gave Boots two injections: Robenacoxib and Doxycycline. He said they would begin to work in a few hours. He also said there’s a pocket of pus in the right eye which is causing the infection to remain.

Ball of pus in the conjunctiva (image courtesy J. Miesle).
I’m to put the antibiotic cream he gave me into it four times a day and to continue giving the Emeraid mixture as often as possible. It’s touch and go now to see if we can turn this infection around. I continued to put either thin mashed potato or dampened Rice Krispies in his beak and syringe the Emeraid Omnivore and Carnivore with vitamins mix into the mouth to help it go down. I give him the Emeraid every 2 hours and the food every 2-3 hours, and I get him up every night around 12 to do this again.
June 7: His appetite has improved and he is up to 78 g. He received more azithromycin from Dr. Dahlhausen and another tube of ophthalmic antibiotic ointment for his eye.
June 14: Every attempt to save his life is being made. We returned to the doctor. The left eye with the cataract is not as red, and the oral tissues are also not as red. He can see a little out of it; I suspect he sees light, and is seeing a little out of the peripheral vision. The ocular bulb will eventually coalesce down till there’s nothing left. The little ball of pus and bacteria is under the bulbar conjunctive tissue, so there will always be something there. Hopefully, it will eventually be absorbed by the body. The doctor just wants to be sure it doesn’t start up the infection once we finish the Azithromycin. He will be on the Azithromycin for 3-8 more weeks. I am to watch the redness in his oral cavity and eyes daily. They seem to be clearing up. He gave me more Azithromycin, and I’m to bring him in every week for the next 3 weeks.
June 21. In for another checkup and more Azithromycin.
June 28. In for another injection of Robenacoxib and Doxycycline
July 6. In for checkup. More eye ointment and another doxy injection. Weight: 89 g. He is stable and continues to eat well. The eye is looking much better.

July 22. The eye is less red and watery. I’m to keep it from closing up by using the antibiotic drops and ointment.
Aug 19. I am to continue putting antibiotic drops and/or eye antibiotic cream into the eye daily. Weight is stable at 89. He is enjoying his food and finding his way around the areas in which he was placed. He can see a little out of the left eye. The circular ridge around the eye is permanent; it is result of the scab pushing the skin away from the eye and impaling the skin.
Oct 22. The eye continues to be in the same condition; however, the tissue in and around the orbit tends to get red when touched. It is extremely thin and fragile. This past week I have noticed very tiny pieces of matter coming out of the orbital area. I remove them with a Q-tip and I notice some moisture coming with them; this makes me sure they are coming out of the orbit. I am continuing to put the sterile drops and ointment on the eye. I believe that little ball of pus in the orbit is breaking down as it appears to be getting smaller. Tiny feathers are beginning to grow on the skin around the circular area.
Nov. 3. Boots’ feather coat is very heavy, and he is beginning to preen more than he had. He is flapping his wings when held out a little better than before. He still doesn’t seem to know how to do this, but we keep working on it. He seems to be seeing a little more than he had with his good eye.
